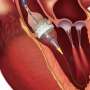
Ross procedure may provide longer survival and better quality of life, study suggests
The Ross procedure, a valve replacement surgery that is largely unused in practice, may provide long-term benefits including longer survival, less clotting and bleeding complications and better quality of life than other valve replacement surgery, finds a study led by researchers at St. Michael's Hospital.
The meta-analysis of existing literature included more than 3,500 adult patients. It found that those who underwent the Ross procedure were 46 per cent less likely to experience death from any cause than patients who underwent mechanical aortic valve replacement.
The Ross procedure is a cardiac surgery where a diseased aortic valve is replaced with the patient's own pulmonary valve. Pulmonary tissue from deceased donors is then used to replace the pulmonary valve. Its use has declined over the past 20 years due to its complexity, potential increased surgical risk and potential risk of follow-up procedures. Mechanical valve replacement is more common, and involves the replacement of the diseased valve with an artificial valve. After the procedure, patients must take blood thinners for the rest of their lives to prevent valve clotting and strokes.
"Our study shows that in contrast to traditional practice, the Ross procedure may be a beneficial option for young to middle-aged adult patients undergoing aortic valve replacement," said Dr. Jan Friedrich, medical director of the Medical-Surgical Intensive Care Unit at St. Michael's and scientist at the hospital's Li Ka Shing Knowledge Institute, who supervised this work along with Dr. Subodh Verma, cardiac surgeon-scientist and director of the CardioLink platform at the Keenan Research Centre for Biomedical Science (KRCBS) of St. Michael's.
Researchers found that in addition to a reduction in death from all causes, patients who underwent the Ross procedure were also 58 per cent less likely to die from valve or heart related causes. This procedure was also associated with lower rates of stroke and bleeding at follow-up, and a higher quality of life.
The meta-analysis found, however, that these patients were 1.7 times more likely to require valve surgery again, likely due to the risks associated with using autograft transplants and the fact that two valves are involved in the Ross procedure instead of one. Researchers note that in current practice pulmonary graft failure is often treated with catheters, avoiding the need to have open heart surgery again.
"Ensuring the best outcomes for patients involves tailoring the surgical approach to the patient," said Dr. Amine Mazine, a cardiac surgery fellow at St. Michael's and lead author of the study. "Superior survival with the Ross procedure is likely due to the ability of a living graft to adapt, but this surgery is not for everyone. It needs to be the right patient undergoing the procedure to ensure the best outcomes."
The meta-analysis was presented this weekend at the European Society of Cardiology Annual Congress in Munich, Germany and published simultaneously in JAMA Cardiology. Dr. Mazine, Dr. Friedrich, Dr. Verma and their team hope this work encourages cardiologists and surgeons to discuss the Ross operation as an option for their young and middle-aged adult patients undergoing aortic valve replacement. They hope it illustrates the potential value of a clinical trial comparing long-term outcomes of the Ross procedure to mechanical valve replacement surgery.
More information: JAMA Cardiology (2018). DOI: 10.1001/jamacardio.2018.2946