Major response to immunotherapy in early-stage mismatch repair deficient colon cancer
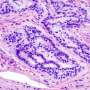
Pre-operative treatment with a combination of the immune checkpoint inhibitors nivolumab and ipilimumab achieves major pathological responses in 100 percent of early-stage colon cancers with mismatch repair deficiencies, according to results reported at ESMO 2018 from the first exploratory phase II trial to investigate this approach.
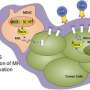
Restoring patients' immune response against cancer cells with checkpoint inhibitors is an established treatment strategy for several tumour types. These agents are of particular interest in mismatch repair deficient (dMMR) tumours because they have high mutational load and upregulation of immune checkpoints.
Checkpoint inhibitors have previously shown durable responses in metastatic colorectal cancers so the new study investigated whether neoadjuvant treatment in dMMR early-stage colon cancer would achieve clinically significant response rates.
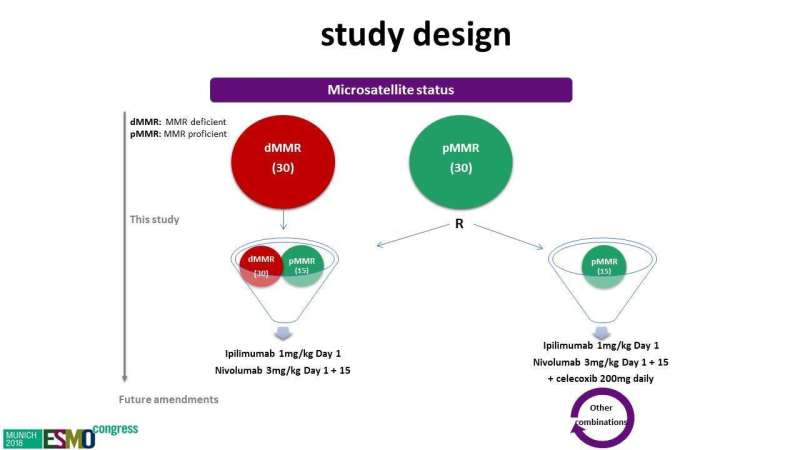
The exploratory trial treated 14 patients with early-stage colon cancer with the checkpoint inhibitors nivolumab (two doses of 3mg/kg on day 1 and 15) and ipilimumab (one dose of 1mg/kg on day 1) before surgery. The two drugs act in different ways to restore immune responses: ipilimumab blocks cytotoxic T lymphocyte associated protein 4 (CTLA-4) and nivolumab blocks programmed cell death protein 1 (PD-1).
Results reported at ESMO 2018 showed that 100 percent (7/7) of the patients with dMMR colon cancer had major pathological responses (defined as <5 percent of viable tumour cells remaining). Four of these seven patients (57 percent) had complete responses.
In contrast, no major pathological responses were seen in pMMR tumours, however there were significant increases in T-cell infiltration.
The immunotherapy regimen was well tolerated and all of the patients underwent radical resection of their tumours without delays in surgery.
"This is the first study with immune checkpoint inhibitors in early stage colon tumours. Our data suggest that neoadjuvant immunotherapy in dMMR colon cancer warrants further research and has the potential to change the standard of care," said lead author Dr. Myriam Chalabi, from the Netherlands Cancer Institute, Amsterdam, Netherlands. She commented: "The response we saw is much more dramatic than in metastatic disease, which we did not expect."
"For MMR deficient tumours, the results were amazing, with 100 percent of patients so far having either complete or near complete responses within the short timeframe of treatment, which is usually 4 weeks," she continued. "I think the finding will have implications for clinical practice in the future. At this stage, it's too early to call it practice changing but it could be if similar results are seen in larger studies."
Commenting on the study for ESMO, Dr. Aurélien Marabelle, Clinical Director of the Cancer Immunotherapy Program at the Gustave Roussy Cancer Centre, Villejuif, France, said: "The study positions immunotherapy at an earlier stage of the disease history for patient with localised disease, and, interestingly, in the neo-adjuvant setting as opposed to the adjuvant setting that is now approved in melanoma and non-small-cell lung cancer."
Marabelle cautioned that the study was small, not randomised and there was no control arm of patients not treated with immunotherapy. He said: "Limited data are available but if they show complete pathological responses in theneoadjuvantsetting, this therapeutic strategy might become standard of carefordMMRcolorectal cancer." He added that dMMR tumours are more frequent in localised cancers (~15 percent of patients) than at the metastatic stage (~5 percent).
Marabelle considered that the finding of some activity with immunotherapy in pMMR tumours in early colon cancer was also potentially interesting. He said: "pMMRCRC does not usually respond to immunotherapy in the metastatic setting. If the researchers find that immunotherapy improves tumour shrinkage preoperatively or reduces post-surgeryrelapse in patients with pMMR early stage colon tumours, this treatment strategy might be of broader interest and impact a lot of patients because of the high frequency of colorectal cancer."
More information: Neoadjuvant ipilimumab plus nivolumab in early stage colon cancer' by Myriam Chalabi during the Proffered Paper Session on Monday 22 October, 11:15 to 12:45 (CEST) in Room 18—Hall A2. Annals of Oncology, Volume 29 Supplement 8 October 2018
Francesco Sclafani. PD-1 inhibition in metastatic dMMR/MSI-H colorectal cancer, The Lancet Oncology (2017). DOI: 10.1016/S1470-2045(17)30512-0