New method uses just a drop of blood to monitor lung cancer treatment
Dr. Tasuku Honjo won the 2018 Nobel Prize in physiology or medicine for discovering the immune T-cell protein PD-1. This discovery led to a set of anti-cancer medications called checkpoint inhibitors, one of the first of which was nivolumab (Opdivo).
Nivolumab helps T-cells fight tumors, however, different patients respond in different ways. It now appears that monitoring the effect of nivolumab on critical immune cells with simple and novel methods may help guide decisions to optimize treatment.
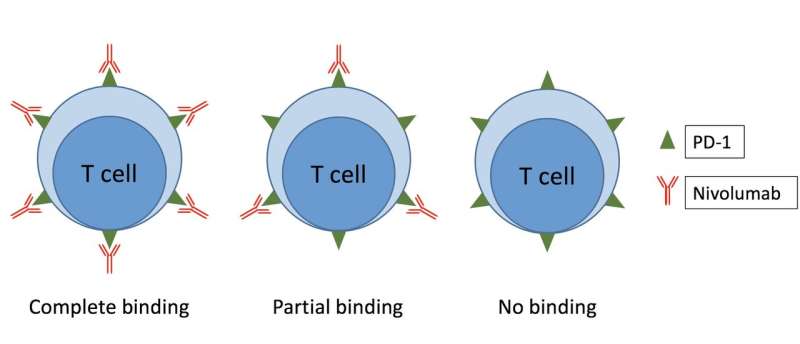
Dr. Shohei Koyama and a team of researchers from Osaka University have devised a simple method for testing the impact of nivolumab in the body. This method measures how nivolumab binds to PD-1 on T-cells weeks after treatment and could provide information needed to monitor treatment more effectively. They recently published their findings in JCI Insight.
The researchers analyzed tiny samples of blood and lung fluid from patients with lung cancer. They measured the amount of nivolumab bound to T-cells, and they also isolated only those T-cells bound by nivolumab to comprehensively analyze cell activation.
The researchers found that the effects of nivolumab on T-cells often persisted in patients for a considerable time after dosing.
"Our simplified method was feasible in real-world patients and demonstrated that nivolumab binds T-cells for more than 20 weeks even after the patient has stopped treatment," study co-author Atsushi Kumanogoh says. "Also, the plasma concentration at which nivolumab stops binding T-cells, and the percentage of bound T-cells, varies from patient to patient."
Their findings also confirmed that the level of T-cell binding does not indicate the functional effect of the drug. A further measure of T-cell proliferation is needed.
"Our findings show that for any given patient we need more information than blood levels of the drug," lead-author Akio Osa says. "It is now clear that we need to measure the amount of nivolumab bound to T-cells and the degree of T-cell proliferation to make treatment decisions. Our method makes this possible with just a drop of blood."
Results from two study participants illustrate the importance of measuring both proliferation and T-cell binding. The first patient showed no response when proliferation was low. In contrast, the second patient showed no tumor growth when proliferation was higher.
"Our combination strategy of monitoring nivolumab binding and the proliferation status of T-cells, is a better way to determine the effect of this drug than monitoring the blood level of nivolumab alone," says co-author Takeshi Uenami.
Overall, understanding in which patients nivolumab has persisting effects over time may be useful for preventing treatment related side effects and guiding the selection of additional therapies.
More information: Akio Osa et al. Clinical implications of monitoring nivolumab immunokinetics in non–small cell lung cancer patients, JCI Insight (2018). DOI: 10.1172/jci.insight.59125