Aftermath of EU referendum linked to rise in antidepressant prescribing in England
Antidepressant prescribing in England rose relative to other types of drug in the immediate aftermath of the results of the European Union referendum in June 2016, when Britons voted in favor of Brexit, reveals research published online in the Journal of Epidemiology & Community Health.
While this finding is open to interpretation, the trend might have been prompted by the increased uncertainty experienced by some sectors of the population, in the wake of the vote, suggest the researchers.
Mental health service provision may need to be strengthened during such periods they add.
When the UK voted to leave the EU on 23 June 2016, the result was unexpected, and considerable uncertainty ensued as to how this would affect the British economy and society, say the researchers.
The evidence suggests that major societal events can affect a nation's mental health, and the researchers wanted to find out if the vote for Brexit might have had a similar impact.
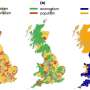
They therefore compared official monthly prescribing data for antidepressants for all 326 voting areas in England with other classes of drugs for conditions less likely to be immediately affected by changes in mood.
These included drugs to treat iron deficiency anaemia, gout, insulins, thyroid problems, drugs to lower blood glucose and blood fats, and muscle relaxants.
The researchers looked at prescribing patterns specifically for the month of July for every year between 2011-16, to capture the immediate aftermath of the referendum result, and across each of those years to see if there were any discernible trends.
To ensure they could compare the different types of drugs, they calculated a 'defined daily dose,' or DDD for short, reached by quantifying the number of milligrams prescribed—derived from the number of pills in a box, multiplied by the strength of each pill.
The 326 voting areas were home to an average of 36.6 general (family doctor) practices, with an average population of 169,534 people in each area.
The number of DDDs prescribed was then divided by each voting area's population to estimate average prescribing levels per head, and these data were then combined with the referendum results for each area.
Analysis of the data showed that before the referendum, DDDs for antidepressants rose during the month of July year on year, as did prescribing for insulins and gout, iron deficiency anaemia, and blood fat and glucose drugs.
In the month after the referendum, DDDs for antidepressants continued to rise, albeit at a slower pace, but those for the other drugs fell, having experienced a period of growth. The only exception were prescriptions for muscle relaxants, which had already been in decline.
The researchers calculated that after the referendum the volume of antidepressants prescribed increased by 13.4 per cent relative to the other classes of drugs studied.
This is an observational study, and as such, can't establish cause. Antidepressants aren't prescribed to everyone, so the results can't be taken to mean that the mood worsened across the whole of England, nor can they rule out that mood actually improved for some people, emphasise the researchers.
"Overall, while our findings point towards a relative increase in antidepressant prescribing as measured by DDDs per capita, results should be interpreted with caution, and further research is needed to examine whether there is any short-term relationship between the referendum result and mental health," they write.
But they say: "Our study focused on an event that was unexpected, leading to an immediate shock. From a more general perspective, this paper shows that shocks nationally can affect health, and that uncertainty about, and expectations of, future effects can have an impact on health in the short term."
And they suggest: "Policies supporting mental health should be intensified in periods of uncertainty."
Policy makers may underestimate the potential costs of Brexit if they focus purely on the impact on the economy or immigration, and ignore any changes in psychological wellbeing that may ultimately affect economic performance and social cohesion, they add.
More information: Journal of Epidemiology & Community Health, DOI: 10.1136/jech-2018-210637