Personalised ultrasound scan showing atherosclerosis helps reduce cardiovascular risk
A new randomised trial of over 3000 people in The Lancet finds that sharing pictorial representations of personalised scans showing the extent of atherosclerosis (vascular age and plaque in the arteries) to patients and their doctors results in a decreased risk of cardiovascular disease one year later, compared to people receiving usual information about their risk.
Smoking cessation, physical activity, statins, and antihypertensive medication to prevent cardiovascular disease are among the most evidence-based and cost-effective interventions in health care. However, low adherence to medication and lifestyle changes mean that these types of prevention efforts often fail.
"Cardiovascular disease is the leading cause of death in many countries, and despite a wealth of evidence about effective prevention methods from medication to lifestyle changes, adherence is low," says Professor Ulf Näslund, Umea University (Sweden). "Information alone rarely leads to behaviour change and the recall of advice regarding exercise and diet is poorer than advice about medicines. Risk scores are widely used, but they might be too abstract, and therefore fail to stimulate appropriate behaviours. This trial shows the power of using personalised images of atherosclerosis as a tool to potentially prompt behaviour change and reduce the risk of cardiovascular disease."
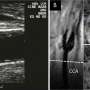
3532 individuals who were taking part in the Västerbotten County (Sweden) cardiovascular prevention programme were included in the study and underwent vascular ultrasound investigation of the carotid arteries. Half (1749) were randomly selected to receive the pictoral representation of carotid ultrasound, and half (1783) did not receive the pictorial information.
Participants aged 40 to 60 years with one or more cardiovascular risk factors were eligible to participate. All participants underwent blood sampling, a survey of clinical risk factors and ultrasound assessment for carotid intima media wall thickness and plaque formation. Each person in the intervention group received a pictoral representation of plaque formation in their arteries, and a gauge ranging from green to red to illustrate their biological age compared with their chronological age. They then received a follow up call from a nurse after 2-4 weeks to answer any questions. The same pictorial presentation of the ultrasound result was also sent to their primary care doctor. Thus, the study had dual targets.
Both groups received information about their cardiovascular risk factors and a motivational health dialogue to promote healthier life style and, if needed according to clinical guidelines, pharmacological treatment.
At one year follow up, the cardiovascular risk score for all participants (3175 completed the follow up) was calculated showing differences between the two groups (Framingham Risk Score decreased in the intervention group but increased in the control group [-0.58 vs +0.35]; SCORE increased by twice as much in control group compared to the intervention group [0.27 vs 0.13]).
Improvements were also seen for total and LDL cholesterol in both groups, but the reduction was greater in the intervention group than in the control group. A graded effect was also noted, with the strongest effect seen for those with the worst results.
"The differences at a population level were modest, but important, and the effect was largest among those at highest risk of cardiovascular disease, which is encouraging. Imaging technologies such as CT and MRI might allow for a more precise assessment of risk, but these technologies have a higher cost and are not available on an equitable basis for the entire population. Our approach integrated an ultrasound scan, and a follow up call with a nurse, into an already established screening programme, meaning our findings are highly relevant to clinical practice," says Prof Näslund.
Importantly, the effect of the intervention did not differ by education level, suggesting that this type of risk communications might contribute to a reduction of the social gap in health. The findings come from a middle-aged population with low to moderate cardiovascular disease risk.
Further research is needed to understand whether the results are sustainable beyond one year, and whether the intervention will lead to a reduction of cardiovascular disease in the long-term. Formal cost-effectiveness analyses will be done after 3-year follow-up.
Writing in a linked Comment, Dr. Richard Kones, Umme Rumana and Alberto Morales Salinas, Cardiometabolic Research Institute (USA), says:
"Despite advances in cardiovascular therapies, coronary heart disease remains the leading cause of death in almost all countries. Two of the most remarkable recent treatments, percutaneous coronary intervention and the availability of proprotein convertase subtilisin/ kexin type 9 inhibitor drugs, have revolutionised cardiology practice. Although life-saving and now essential therapies, whether they will be able to reduce the incidence and associated morbidity and mortality of coronary heart disease remains unlikely since the increase in prevalence of obesity and diabetes is raising the background level of cardiovascular risk... Although there are proven methods of lowering cardiovascular risk and these are generally being better used generally in high-income countries, poor adherence and uneven availability and access in low income and middle-income countries still pose serious challenges... About less than half of all patients taking medications are adherent, which substantially increases morbidity and mortality. Non-adherence to medication accounts for 33-69% of all hospital admissions in the USA, and, among patients with coronary heart disease, the extent of low adherence is related to the number of adverse cardiovascular events. Poor adherence is multifactorial and can broadly be grouped into categories related to patients, physicians and therapies, communication, health-care systems, socioeconomic factors, and unpredictable negative effects of the internet. One of the most pertinent factors is patient-related perceived risk and motivation. Despite the many methods that have been proposed, effectiveness in improving adherence and outcomes has been relatively disappointing. It is in this context that the randomised controlled trial by Ulf Näslund and colleagues in The Lancet is relevant."
More information: The Lancet (2018). www.thelancet.com/journals/lan … (18)32818-6/fulltext