Cracking the code on 'cavernous malformations'
Although most have never heard the term "cavernous malformation," as many as 1 in 500 people may have this condition, which can cause bleeding, seizures, muscle weakness, and motor and memory problems.
"Cavernous malformations are rare—even to a neurologist or neurosurgeon," says Dr. Kelly Flemming, a Mayo Clinic neurologist. "Having coordinated care by providers familiar with the disease is very important to patients."
To that end, the Angioma Alliance named Mayo Clinic a Center of Excellence in 2017. The center treats and conducts research on cerebral cavernous angiomas, which go by many names, including cerebral cavernous malformations, cavernous hemangiomas and cavernomas.
Dr. Flemming is medical director of the effort, and Mayo patients like Kandie Nelson of Sioux Falls, South Dakota, are helping, too.
"I was working at the front desk at a hotel," explains Kandie Nelson. "And I went to answer the phone, and it came out, 'Blah, blah, blah.' I just—I couldn't talk. And my hands and my feet started going numb. And, then, I fell to the ground."
Kandie was rushed to the hospital and eventually was diagnosed with a cavernous malformation.
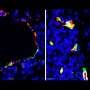
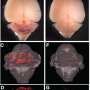
"They look like this little raspberry or cluster of grapes in the brain," says Dr. Flemming.
A cavernous malformation happens when tiny capillaries divide abnormally and create a small tangle of blood vessels. Many who have the condition don't know it, since symptoms are rare.
"We find these accidentally," Dr. Flemming adds. "Somebody had a head trauma, and they are being scanned, looking for trauma, but we incidentally find one of these. Or they may have migraines, and they undergo an MRI."
"They can just kind of blow out, and that can cause a hemorrhage in your brain," Kandie adds.
"Quite often, there is displacement rather than destruction of the surrounding tissues, and that's the reason why many patients can have even a significant, fairly large bleed without having major symptoms," says Dr. Giuseppe Lanzino, a Mayo Clinic neurosurgeon. "This is also the reason why many patients, after a symptomatic bleed, can have some degree of improvement."
Dr. Lanzino says surgery to remove one of these malformations is considered only when it's causing problems—as was the case for Kandie.
"It's very close to the surface of the brain, so it would be very easy to get to. So we opted for that," says Kandie, explaining the decision she made with doctors about her malformation.
"If it's in a difficult place, like deep inside the brain or in the brain stem, then typically we would wait and watch and only do surgery if there was a second bleed or increasing symptoms," adds Dr. Flemming.
It's still unclear why most people develop these malformations. But in about 20 percent of cases, there's a family connection. That's true for Kandie.
"So my children had 50 percent chance of having it," she explains.
And two of them do, including her son, Bryan Nelson.
"They're usually in the brain or the brain stem," Kandie said. "But he had one in the spinal cord."
Bryan had that cavernoma removed just weeks before his high school graduation. Kandie says a second malformation on Bryan's brain stem later affected his ability to walk and talk.
"He was kind of slurring his words," she adds, explaining Bryan's symptoms.
"In his case, we were able to remove the cavernous malformation from the brain stem, along with the fresh blood that was there from the recent bleed, and he was able to make quite a remarkable recovery," Dr. Lanzino says.
"My scar starts right here—then behind my ear," says Bryan's sister, Kayla Nelson, as she pointed to the location of her surgery.
Kayla's cavernous malformation struck in a different way.
"I was going up the stairs," Kayla adds. "I remember kind of going into a seizure. So I had texted my mom and told her what had happened. And she was, like; 'All right—yep, you're going to the Mayo Clinic. I'm making an appointment now.'"
"It was in a particular location in the brain called the temporal lobe, which is common for any type of abnormality to provoke seizures," Dr. Flemming says. "And even though she went on seizure medications, she was still having them. And, so, if people are having recurrent seizures, despite trials of medications, then surgery would be recommended there, as well."
Kayla became the third member of her family to undergo surgery and find relief from cavernous malformation.
"My seizures are gone," says Kayla.
"I think a lot of patients I talk to—they struggle with finding people with the correct expertise to answer a lot of their questions," Dr. Flemming says.
"At the center here at the Mayo Clinic, we have expertise in all different areas, including the diagnosis—both clinical and imaging—the surgical treatment and the nonsurgical treatment of cavernous malformations," adds Dr. Lanzino.
And, thanks to families like the Nelsons, that expertise continues to deepen.
"All three of us have donated our malformations to science," Kandie explains. "Hopefully, they can try to figure out how they grow and what they can do to stop them from growing. God puts you here for a reason. I believe one of my reasons is to help find a cure for this."
©2019 Mayo Foundation for Medical Education and Research
Distributed by Tribune Content Agency, LLC.