August 13, 2019 feature
Application of hydroxyapatite nanoparticles (n-HA) in tumor-associated bone segmental defect
Materials scientists widely incorporate hydroxyapatite (HA) for bone repair in bone tissue engineering (BTE) due to its superior biocompatibility as a natural component of human bones and teeth. In a recent report on Science Advances, a research team highlighted the proliferation-suppressive effect of HA nanoparticles (n-HA) against a variety of cancer cells by combining the translational value of n-HA as a bone-regenerating material and an anti-tumor agent. In the study, Kun Zhang and an interdisciplinary research team in the departments of Orthopedic Surgery, Dermatology, Biomedical Metal Materials and the National Engineering Research Center for Biomaterials in China, demonstrated the inhibition of tumor growth, metastasis prevention and the enhancement of the survival rate in tumor-bearing rabbits treated with n-HA.
They confirmed activation of the mitochondrial-dependent apoptosis pathway in vivo and observed a stimulated immune response to n-HA induced antitumor effects. The research team then loaded a porous titanium scaffold with n-HA and implanted it into a critical-sized segmental bone defect in a rabbit tumor model for translational studies. Based on the results, they verified the ability of the n-HA releasing scaffold to suppress tumor growth and osteolytic lesion while promoting bone regeneration. The research findings provide a strong rationale to use n-HA to regenerate tumor-associated bone segmental defects in vivo.
In the United States, approximately 2,500 new cases of primary bone cancer are diagnosed annually with approximately half the patients exhibiting bone metastasis. During standard clinical treatment of bone cancers, the surgical approach includes resection and reconstruction of the affected bone, followed by adjuvant radiation or chemotherapy. Although load-bearing artificial implants are currently adopted in clinical practice, poor implant-bone osseointegration and the difficulty of new bone formation in a tumor environment remain major challenges for orthopedic surgeons. Incomplete surgical resection of the affected tissue can also risk the spread of tumor cells to result in 8 percent recurrence or metastases. As a result, researchers urgently aim to develop an implant that combines antitumor activity and bone regeneration functions.
Since the 1970s, clinicians have applied HA-based biomaterials clinically during orthopedic and dental repair. Materials scientists have also developed surfaces modified with HA as prosthetic metal implants for enhanced bone integration. Notable research studies have shown the capacity of n-HA to inhibit cancer cell proliferation and induce apoptosis, including osteosarcoma cells, breast cancer cells, colon cancer cells and liver cancer cells, while sparing normal cells. Preceding studies provided insight to the mechanism of n-HA antitumor activity based on in vitro experiments, although much remains to be known of the underlying mechanism in vivo.
Testing the new experimental strategy in the lab
In the present work, Zhang et al. presented an unprecedented strategy to combine bone tumor treatment using a 3-D printed titanium scaffold modified with n-HA for antitumor function. They conducted in vitro co-culture experiments first, to demonstrate the ability of the synthetic, rod-shaped n-HA to induce apoptosis in the malignant VX2 tumor cells. Thereafter, the research team implemented an intramuscular tumor model in immunocompetent rabbits to show the suppression of tumor development and reduced metastasis.
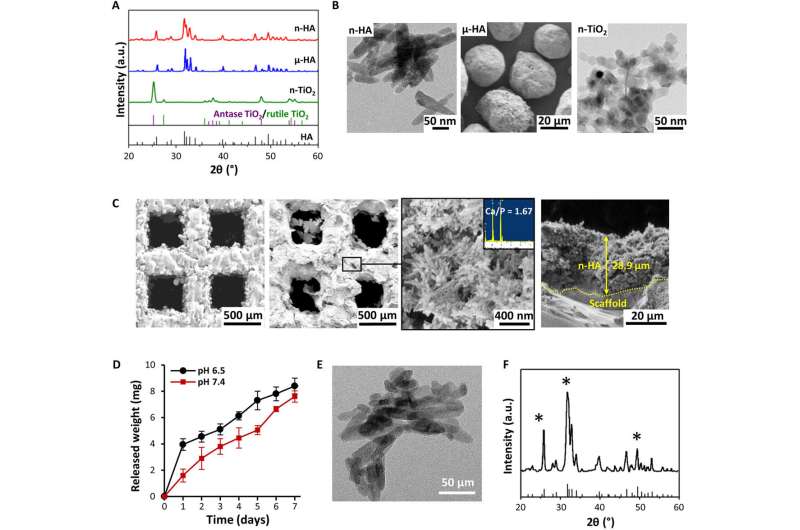
Researchers initially observed and reported the anti-tumor effect of n-HA in 1993, when they serendipitously found a control group of pure n-HA to inhibit Ca-9 cancer cell lines further validated in 2003 using functional studies in vitro. In the present work, Zhang et al. used µ-HA and n-TiO2 particles as control groups alongside n-HA to determine if the antitumor effect originated from the material composition or particle size. For this, they used X-ray diffraction analysis (XRD) and confirmed similarities of the HA phase composition between n-HA and µ-HA. Then using transmission electron microscopy (TEM) images they revealed the rod shape of n-HA and used scanning electron microscopy (SEM) micrographs to observe µ-HA.
They then engineered porous titanium scaffolds using selective laser sintering to satisfy the load-bearing requirements for rabbit cortical bone replacement. Zhang et al. enhanced the bioactivity of the printed scaffolds using acid-alkali treatment and achieved n-HA coating using a combined method of slurry foaming and impregnation. The scientists characterized (tested) the scaffolds to determine the surface chemistry and kinetics of n-HA release in an acidic environment.
Testing the biocompatibility and cancer cell apoptosis with different particles.
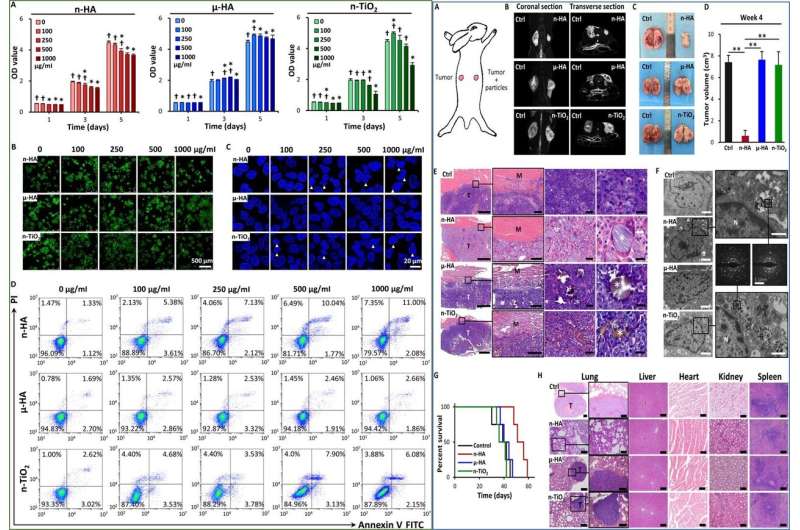
To test in vitro antitumor activity and toxicity of the particles, the researchers chose a wide range of n-HA concentrations to co-culture with VX2 tumor cells or normal L929 fibroblast cells. During prolonged experiments n-HA reduced the viability of tumor cells, although comparatively, µ-HA did not reduce the viability of either cell type, while n-TiO2 decreased the viability of VX2 and inhibited L929 cell growth with prolonged time.
When Zhang et al. tested the in vivo antitumor ability of n-HA, they used an intramuscular VX2 tumor model on both flanks (right and left) of the rabbit, and administered n-HA, µ-HA and n-TiO2 on either side. By week three, they used magnetic resonance imaging (MRI) of individual animals to show reduced HA-treated tumor size in the right hand side, compared to the control in the left hand side. Comparatively neither µ-HA nor n-TiO2 showed tumor growth suppression in vivo during the same period.
The scientists harvested the tumor samples at week 4 to confirm the antitumor ability of n-HA using histological staining at the interface of the tumor and muscle tissue. They noted diverse immune cells surrounding the n-HA particles, such immune diversity was not observed surrounding µ-HA and n-TiO2 coated scaffolds. Using TEM observations, Zhang et al. showed both n-HA and n-TiO2 internalized within tumor cells. Histological findings at week 4 indicated the prevention of metastasis to the lung with n-HA animal groups, although similar observations were not recorded with µ-HA or n-TiO2. Metastasis elimination in rabbits treated with n-HA led to longer survival rates and lower rates of tumor positive cells compared to those treated with other materials.
Investigating the anti-tumor mechanisms of n-HA
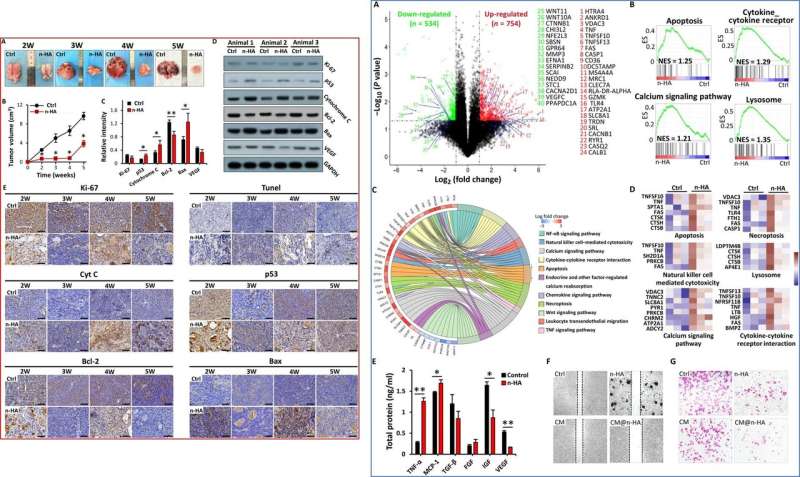
After several weeks, the scientists analyzed the mitochondrial apoptosis pathway activation of the tumor tissue by n-HA using immunohistochemistry (IHC), nitric oxide synthase experiments and protein expression studies using Western blotting. They observed reduced protein expression of Ki-67 and increased expression of TUNEL (terminal deoxynucleotidyl transferase) for reduced cell proliferation and induced apoptosis. They also noted higher expression of the p53 protein in the n-HA group in response to cellular stress to suppress oncogenesis. And observed a significant increase for n-HA induced Bcl-2 associated X protein (BAX) – a proapoptotic protein while lowering Bcl-2 an anti-apoptotic protein in the mitochondrial apoptotic pathway. Together, the proteins regulated the release of proapoptotic factor cytochrome C (cyt C) from the mitochondria into the cytosol for cell apoptosis.
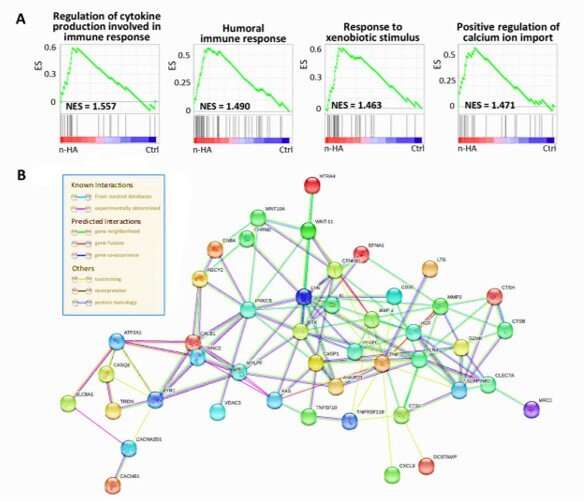
Zhang et al. further investigated potential antitumor mechanisms of n-HA by performing an mRNA expression profile microarray and confirmed the expression of several genes using qRTPCR (quantitative reverse transcription polymerase chain reaction). They found that n-HA significantly upregulated the expression of tumor apoptosis related genes; suggesting the activation of the extrinsic death receptor apoptosis pathway via n-HA. The scientists identified multiple mechanistic pathways using databases such as Kyoto Encyclopedia of Genes and Genomes (KEGG) and Gene Ontology (GO). The results showed the influence of n-HA interference on multiple aspects of the tumor microenvironment to suppress tumor promoting functions.
Conducting segmental bone defect repair with n-HA/scaffolds in a tumor environment
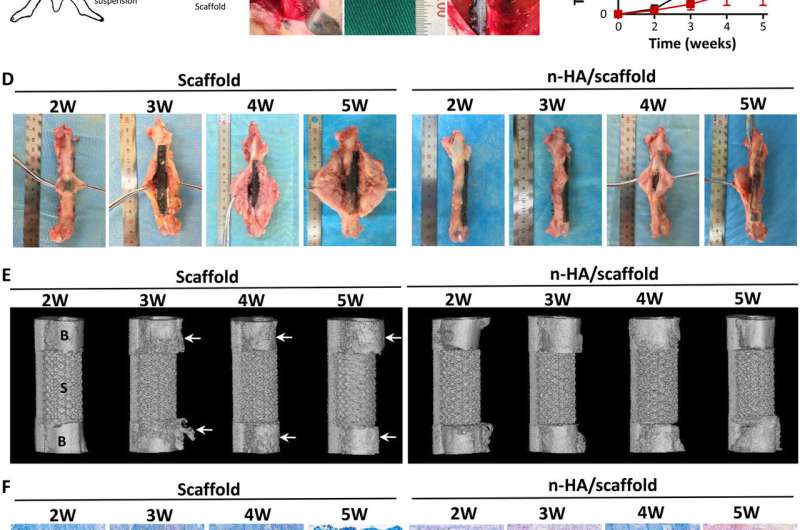
The scientists then completed wound healing assays to identify if secretory inflammatory cytokines such as TNFα (Tumor Necrosis Factor Alpha) were released from macrophages as a result of n-HA stimulation to inhibit tumor cell migration. They confirmed that cytokine secretion by macrophages upon stimulation with n-HA could decrease tumor cell migration. When the research team completed segmental bone defect repair with a n-HA/scaffold in a tumor microenvironment of a rabbit model thereafter, they observed a 73.8 percent reduction in the tumor volume of rabbits with the n-HA loaded scaffold implant. Histological studies showed the pores of the empty scaffold filled completely with tumor cells, while fewer tumor cells aggregated in the n-HA/scaffold. The n-HA coated implants suppressed tumor growth and promoted bone regeneration with ability to eventually dissolve into calcium and phosphorous ions for gradual replacement by new bone in vivo.
In this way, Kun Zhang and colleagues established a rabbit femur bone tumor model with VX2 and demonstrated the n-HA coating effects in tumor growth suppression, alongside their safety for bone regeneration relative to normal cells and tissue. Although the results are promising in a translational animal model, the effects of n-HA in a clinical environment remain to be determined. The research team will launch clinical trials with n-HA coated hydrogels for post-surgical cancer treatment for promising clinical outcomes of biosafety and anti-tumor capabilities. They then aim to implement a series of n-HA shape/crystallinity-dependent experiments to comprehend the compound's mechanism of action, based on the diverse physical and chemical properties of n-HA variants.
More information: Kun Zhang et al. Application of hydroxyapatite nanoparticles in tumor-associated bone segmental defect, Science Advances (2019). DOI: 10.1126/sciadv.aax6946
Yingchao Han et al. Different Inhibitory Effect and Mechanism of Hydroxyapatite Nanoparticles on Normal Cells and Cancer Cells In Vitro and In Vivo, Scientific Reports (2014). DOI: 10.1038/srep07134
J. Yang et al. The enhanced effect of surface microstructured porous titanium on adhesion and osteoblastic differentiation of mesenchymal stem cells, Journal of Materials Science: Materials in Medicine (2013). DOI: 10.1007/s10856-013-4976-4
© 2019 Science X Network