Hot flashes shown to be linked to increased risk of later cardiovascular disease events
Previous studies suggested an association between hot flashes and cardiovascular (CVD) disease. But little research linked hot flashes to "hard" clinical CVD events like heart attacks and strokes. A new study measuring clinical CVD outcomes presents the strongest evidence of frequent or persistent hot flashes associated with higher CVD event risk. Study results will be presented during The North American Menopause Society (NAMS) Annual Meeting in Chicago, September 25-28, 2019.
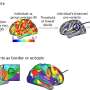
Most studies that have previously attempted to link hot flashes with an increased risk of CVD have relied on subclinical measures of CVD, which are proxies for clinical CVD, but not actual events. They have also relied upon recalled measures as hot flashes from years earlier, which can be biased by memory. The Study of Women's Health Across the Nation (SWAN), a longitudinal 20-year study of the menopause transition, is uniquely positioned to confirm this link because it assessed hot flashes regularly throughout the menopause transition and has also collected information on CVD events as women age.
In this latest study based on SWAN data, researchers tested whether the hot flashes early in the transition or persistent hot flashes over the transition impacted incident CVD risk. They found that frequent, as well as persistent, hot flashes over the menopausal transition translated into a higher risk of having a CVD event in the future. They additionally discovered that this association was not explained by standard CVD risk factors. In fact, frequent hot flashes at the beginning of the study were associated with a doubling of risk of clinical CVD events, and persistent hot flashes over the study with an 80% increased risk of clinical CVD events in the subsequent 20 years.
"This is the strongest test of whether hot flashes are associated with actual clinical CVD events, such as heart attacks and strokes, which represent the most clinically relevant outcome," says Dr. Rebecca Thurston, lead author of the study from the University of Pittsburgh. "It's the strongest because we measured hot flashes prospectively multiple times over the course of the menopause transition, which is different than most other studies of CVD events that ask women to recall their hot flashes over months or years. We also had measures of clinical CVD events, rather than other proxy measures. We brought these data together to address this important question in a more rigorous fashion than prior studies."
"With heart disease being the number one killer of women, it's critical that we understand its many different risk factors in order to help create more preventative and treatment strategies for women transitioning through menopause," says Dr. Stephanie Faubion, NAMS medical director.