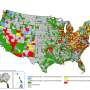
Barrier to rural opioid treatment: Driving distance to methadone clinics

People who live in rural counties in five states heavily affected by the opioid epidemic must drive longer distances to obtain methadone, a treatment for opioid addiction, compared to individuals from urban counties, say Yale researchers. Their study, published in the Journal of the American Medical Association (JAMA), suggests these long drive times in rural counties could be reduced by making methadone more accessible in primary care clinics, they said.
In the United States, methadone for opioid addiction can only be dispensed by clinics certified by the federal government as Opioid Treatment Programs, or OTPs. This requirement, combined with state and local laws, limits the number of clinics offering methadone for opioid addiction despite a need for methadone in all communities. Given the shortage of OTPs, a Yale research team focused on drive times to OTPs in both rural and urban counties in five states: Indiana, Kentucky, Ohio, Virginia, and West Virginia.
Using a tool that is similar to common smartphone map apps, the researchers calculated the minimum drive times from the population center of a county to the nearest OTP or methadone clinic. They also calculated drive times to Federally Qualified Health Centers (FQHCs), community-based primary care clinics, to examine how dispensing methadone in these clinics would impact drive times. Finally, they calculated drive times to dialysis centers to compare driving distance to methadone versus to treatment for kidney disease.
The researchers found that mean drive times to OTPs compared to the other centers were longer in all counties, with the exception of the largest cities. The mean drive time to a methadone clinic was 37 minutes compared to 16 and 15 minutes for FQHCs and dialysis centers, respectively. But the driving time to methadone was greatest in rural areas; the longest drive time was nearly two hours.
"People who live in rural counties face long drive times to access methadone, and this barrier to treatment could be reduced if methadone prescribing occurred at Federally Qualified Health Centers," said corresponding author Paul Joudrey, M.D.
This difference in distance to treatment centers is significant because by law, methadone treatment uniquely requires six visits per week to get the medication, while dialysis treatment for kidney disease typically involves three visits, the researchers noted.
"This study makes clear how poorly accessible methadone is for rural communities harmed by the opioid epidemic," said Joudrey. The five states studied contain the highest county rates of opioid-related overdose deaths.
While another drug, buprenorphine, is used in primary care settings as well as OTPs to treat opioid addiction, it does not work for everyone, he noted. Addiction experts agree that methadone should be available in all communities as an important treatment option to improve health and reduce death among people with opioid addiction.
Potential solutions to this barrier to treatment could include policy changes to support dispensing of methadone for opioid treatment at FQHCs, construction of new methadone clinics, or integration of methadone into primary care, the researchers said. By contrast, in Canada and Australia, methadone can be prescribed by certified primary care providers and dispensed by community pharmacists.
More information: JAMA (2019). DOI: 10.1001/jama.2019.12562