Worried about brain lesions and dementia? Check this blood pressure number
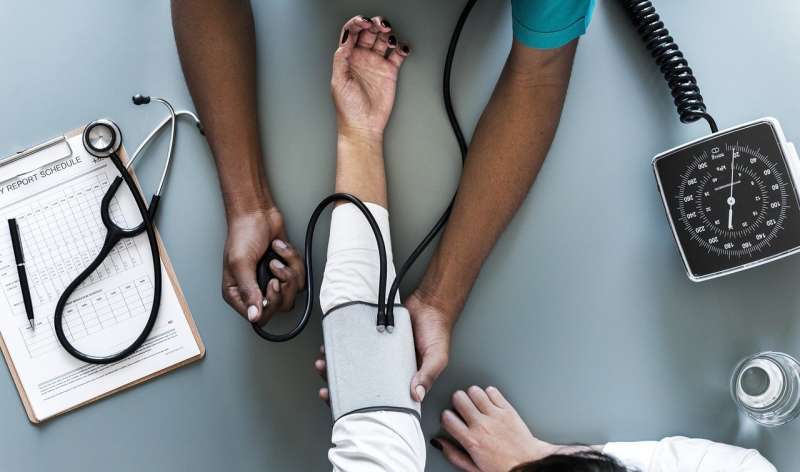
The top number on a blood pressure test is widely viewed as the best gauge of a person's overall risk for heart disease. But the bottom number could be important when it comes to evaluating the chance of a person having scars on their brain that could be an indicator for dementia, stroke or falls.
Researchers in a new study looked at the link between blood pressure scores and the number and location of these brain scars, called white matter lesions. In 1,205 women and men who were 50 and older—two-thirds of whom were Hispanic—the investigators found those with the lowest diastolic blood pressure (the bottom number) had fewer white matter lesions on MRI scans than those with higher diastolic blood pressure.
Michelle R. Caunca, a medical student at the University of Miami Miller School of Medicine who led the study, said the team had expected to find systolic blood pressure (the top number) was associated with white matter lesions. Other studies have shown people with high systolic blood pressure are more likely to have the narrowed arteries that cause these lesions, she said.
Yet the new study, published Wednesday in the American Heart Association journal Stroke, found people with diastolic blood pressure lower than 80 had smaller white matter lesions in three regions of the brain seen on MRI compared to people with diastolic blood pressure over 90.
"Different regions are supplied by different vessels, and certain (diseases) affect certain regions in different ways," said Caunca. "Looking at different regions allows us to explore, in an indirect way" how blood pressure might affect the brain's blood vessels.
"This focus on distinct regions is a new contribution to the literature," said Dr. Rebecca Gottesman, a professor of neurology and epidemiology at Johns Hopkins University in Baltimore who was not involved with the research.
"The specific relationship with periventricular (region) white matter lesions is important because these lesions tend to be more strongly associated with cognitive problems," she said.
Systolic blood pressure indicates how much pressure a person's blood exerts against the artery walls when their heart beats. Diastolic blood pressure indicates how much pressure a person's blood exerts against the artery walls while their heart rests between beats.
People with a diastolic blood pressure reading of 80 or higher are considered to have high blood pressure, according to guidelines from the American College of Cardiology and AHA.
White matter is composed of nerve fibers that transmit messages to and from the brain that help guide muscle movement, sensation and thinking. Lesions can block these messages, increasing the risk for falls. These lesions also increase a person's risk of having a stroke or developing problems with thinking and memory.
By age 60, between 10% and 20% of people have white matter lesions, according to an AHA scientific statement about silent cerebrovascular disease. They are seen in most adults over age 90.
Caunca said although the association with diastolic blood pressure was not expected, it was consistent with other studies.
Gottesman said the new study "provides further evidence that it is important to know your blood pressure and talk to your doctor about the best treatment for you."
It also shows, she said, "the importance of the diastolic blood pressure, which is less typically considered when decisions are being made about treating patients with hypertension."
More information: Michelle R. Caunca et al. Diastolic Blood Pressure Is Associated With Regional White Matter Lesion Load, Stroke (2020). DOI: 10.1161/STROKEAHA.119.025139
Paul K. Whelton et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines, Hypertension (2017). DOI: 10.1161/HYP.0000000000000065
Eric E. Smith et al. Prevention of Stroke in Patients With Silent Cerebrovascular Disease: A Scientific Statement for Healthcare Professionals From the American Heart Association/American Stroke Association, Stroke (2016). DOI: 10.1161/STR.0000000000000116