Critically injured soldiers have high rates of mental health disorders
U.S. combat soldiers who suffered a moderate or severe traumatic brain injury (TBI) are more likely than soldiers with other serious injuries to experience a range of mental health disorders, according to a new retrospective study by University of Massachusetts Amherst health services researchers.
"A central takeaway is that severe TBI is associated with a greater risk of mental health conditions—not just PTSD," says lead investigator David Chin, assistant professor of health policy and management in the School of Public Health and Health Sciences. "Our findings suggest that patients who are critically injured in combat and sustain severe TBI have particularly high rates of mental health disorders."
The research, published in the journal Military Medicine, is the largest and broadest look at severe combat injury in the military and associated mental health outcomes. Chin and co-author John Zeber, UMass Amherst associate professor and program head of health policy and management, examined the cases of 4,980 military members—most from the Army or Marines—who were severely injured during combat in Iraq and Afghanistan between 2002 and 2011. Nearly a third of them suffered moderate or severe TBI.
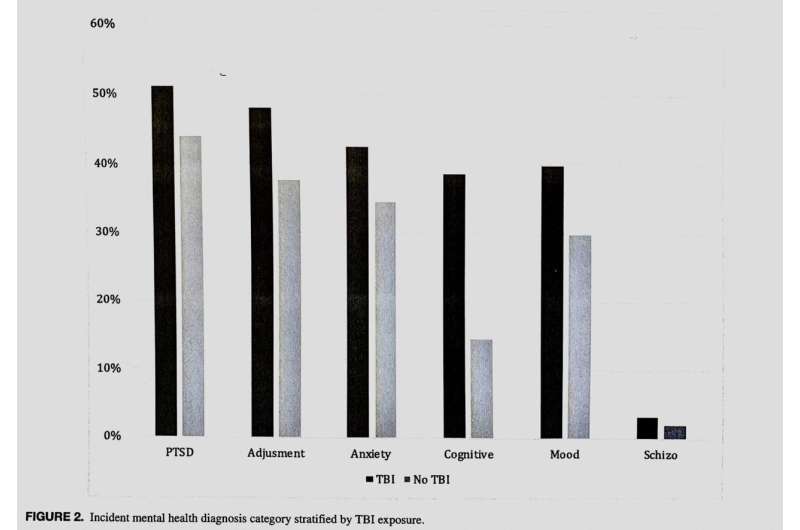
Mining data from the U.S. Department of Defense, Chin found that 71% of all the severely injured soldiers were diagnosed in follow-up care with at least one of five mental health conditions: post-traumatic stress disorder (PTSD), anxiety and mood disorders, adjustment reactions, schizophrenia and other psychotic disorders, and cognitive disorders. Previous research reported that a much lower 42% of seriously injured combat soldiers went on to be diagnosed with mental health disorders. And Chin notes that his study defined mental health diagnoses more narrowly.
In Chin's research, diagnoses for every mental health condition were higher among the cases of TBI than other severe injuries.
"Most of the research on TBI has looked at mild to moderate brain injury," Chin says, with estimated incidence of associated PTSD to be as high as 23% - significantly lower than the 46% incidence Chin's research noted in cases of more severe TBI.
In addition, Chin found that the risk for post-traumatic stress disorder (PTSD) is higher—not lower, as previous investigators have assumed—among combat soldiers with more severe TBI.
"There was a common belief that having a severe TBI resulted in an amnestic effect on PTSD—the injuries were so severe that the patients have no memory of the event and that put them at lower risk of having mental health outcomes. This data showed to the contrary," Chin says.
In addition to including personnel from all four military service branches, the study followed the soldiers' care for a median period of more than four years. Earlier studies about TBI in the military typically involved one service branch and only followed the soldiers for one year after the injury.
Even with the longer timeframe, Chin says the study "definitely underestimates" the prevalence of mental health conditions among severely injured soldiers. Among the study's limitations: researchers had access only to Department of Defense-related records, so researchers were unable to track cases after the soldiers were discharged; and the military culture engenders an underreporting of mental health symptoms.
While Chin emphasizes that more research is necessary, the study illustrates the importance of monitoring the mental health status of seriously injured soldiers, especially those with severe TBI, for years after their injury, and ensuring that clinical and support services are available to veterans and their families.
More information: David L Chin et al, Mental Health Outcomes Among Military Service Members After Severe Injury in Combat and TBI, Military Medicine (2019). DOI: 10.1093/milmed/usz440

















