IVF twins: two hearts, quadruple the risk
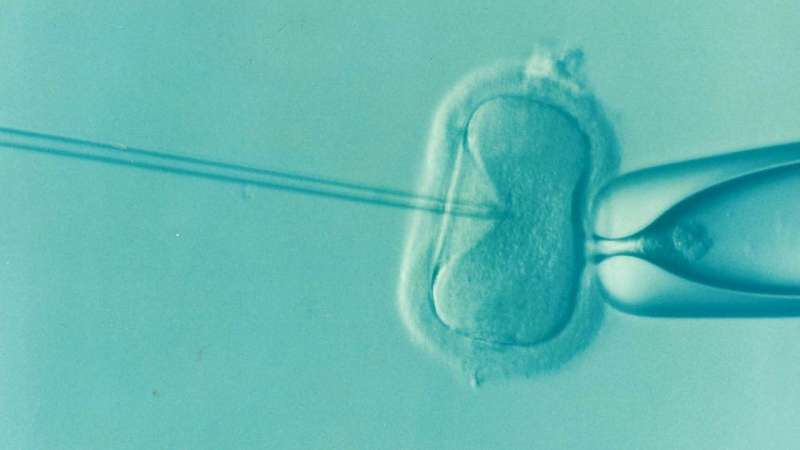
Twins born through IVF have quadruple the chance of having a congenital heart problem, according to research emerging from South Australia.
Professor Michael Davies from the University of Adelaide's Robinson Research Institute has collaborated on a new study with global implications, analyzing more than 500,000 births in Ontario, Canada, with the results published in the journal JAMA Pediatrics.
The findings build on Australian research showing that having a baby as a result of using assisted procedures such as In-Vitro Fertilisation (IVF) nearly doubles the chance that a baby will have heart problems.
The new research showed about 85 per cent of the excess risk around congenital heart defects related to twins.
"This risk appears to double again for twins compared to singletons," Prof Davies said.
"Globally, this is important as the chance of a twin pregnancy is highly influenced by clinical and patient treatment choices."
The findings, Prof Davies said, were particularly important to share as the extra risk associated with having twins through IVF was preventable.
The findings also support work in Australia initiated by Prof Davies where IVF patients were provided new recommendations about the higher risks associated with having twins.
This in turn dramatically reduced the chance in Australia of having twins through infertility treatments as more patients and clinicians opted for single embryo transfers.
"The number of single embryo transfers doubled very quickly in the early 2000s when our Australian research confirmed the safety and effectiveness of this option," Prof Davies said.
Currently, 4 per cent of pregnancies are conceived using assisted reproductive technology with upward trends in recent years.
"Multiple embryo transfer slightly improves the chance of pregnancy but can increase the chances of twins being born by 10 times," Prof Davies said.
"This has reached epidemic levels in many places including North America because of the cost of treatment."
Australia has a lower out-of-pocket cost of an IVF cycle at approximately AU$5000 than many other countries, and among the lowest rate of twins being born after IVF treatment of about four percent.
This compares to 20 per cent of births in IVF being twins in North America where one embryo transfer costs approximately US$20,000 with the patient often being responsible for the full cost.
About 15 in every 1000 babies in Australia are born with a congenital heart defect including narrowing of the arteries, holes in the walls that separate the chambers of the heart and an undeveloped heart.
A heart defect is a major cause of death and disability in the first year of life.
Dr Shi Wu Wen and Dr Mark Walker of the Ottawa Hospital and the University of Ottawa led the most recent study where Prof Davies collaborated, having established a joint PhD program with Ottawa University at the beginning of last year.
The study examined records of congenital heart defect diagnoses with reproductive technology cycles in 507,390 singleton or twin pregnancies (10,149 assisted pregnancies and 497,241 non assisted pregnancies) including singleton and twin early pregnancy losses, stillbirths and live birth in Ontario between 2012 and 2015.
"This study provides further support for the practice of limiting the number of embryos transferred during in vitro fertilization and similar techniques," Dr Shi Wu Wen said.
More information: Shi Wu Wen et al. Associations of Assisted Reproductive Technology and Twin Pregnancy With Risk of Congenital Heart Defects, JAMA Pediatrics (2020). DOI: 10.1001/jamapediatrics.2019.6096



















