The doctor gap: In rural America, it's all hands on deck

Dr. Jennifer Cobanov had been tracking her young thyroid patient for years. The girl's antibody levels were elevated, but her thyroid functioned normally. Then, routine blood work revealed something quite unusual: Her underactive thyroid had suddenly switched into overdrive.
Last November, the California pediatrician referred the 13-year-old to a specialist at Loma Linda University Children's Hospital, the nearest major medical center. The girl's mother booked the soonest available appointment—for this spring.
Why the long wait? In California's Inland Empire, a huge swath of the state that includes San Bernardino and Riverside counties, pediatric subspecialists are hard to come by. The region suffers from a severe shortage of both primary care doctors and specialists.
Janet Coffman, a health workforce researcher at the University of California, San Francisco, said there are several reasons for the doctor gap. For one, the massive area encompasses both low-income urban pockets and vast rural expanses.
"People in the rural areas struggle more with access to specialists, as is typical of what you'd find in rural areas across the U.S.," she noted.
When Coffman and her colleagues studied the state's physician supply for the California Health Care Foundation, specialty doctors serving the Inland Empire, at 64.3 per 100,000 residents, ranked well below most other areas of the state. For example, the affluent Bay Area had more than twice as many specialists. As for primary care, the gap was equally dismal. Riverside/San Bernardino had 34.5 doctors per 100,000 people. That's just slightly more than half the number serving the Bay Area.
Doctors are scarce, need is huge
Twenty percent of the U.S. population resides in rural areas of the country, but only 11% of physicians practice there, according to the National Rural Health Association.
How can that be?
Along with general forces influencing physician supply and demand, experts point to other factors: doctors not wanting to live in rural areas; subspecialists choosing to practice in cities with large potential pools of patients; and a dwindling number of med school applicants with roots in rural America.
It doesn't help that rural hospitals are closing at an alarming rate. Researchers at the University of North Carolina at Chapel Hill report that at least 124 hospitals in rural areas have closed since 2010. Such closures are associated with decreases in the supply of both primary care physicians and specialists, according to a December 2019 paper in the journal Health Affairs.
In rural communities, driving 10, 50 or even 100 miles to see a doctor is not uncommon. Carol (not her real name), a former health professional in her mid-50s, suffers from complex heart and neurological issues. She and her husband must leave their rural New York home three hours in advance of each specialist appointment to make it to Manhattan on time.
But the specialists she needs to see are not located in her town. When specialty care is difficult to access, people can suffer real health consequences.
Another study in the same issue of Health Affairs sheds light on rural/urban disparities among Medicare beneficiaries with chronic conditions. Patients in rural areas have a 40% higher rate of preventable hospitalizations and a 23% higher death rate than their urban counterparts.
Then researchers considered things like how sick and frail people were, whether they were living in poverty, and how much education they had—all of which are known to affect people's health outcomes. After adjusting for those variables, seeing a specialist was associated with a nearly 16% lower rate of preventable hospitalizations and a 16.6% lower death rate.
"So whether you're urban or rural, if you have a chronic condition, it's good for you to see a specialist," said Kenton Johnston, an assistant professor of health management and policy at Saint Louis University and the lead author on the Health Affairs research.
How much of a difference does seeing a specialist make? "A pretty big chunk," Johnston observed. Access to specialists accounts for 55% of the difference in the rate of preventable hospitalizations and 40% of the difference in the death rate.
If you're someone who has heart failure, seeing a cardiologist "might keep you out of the hospital and keep [you] alive longer," he reasoned. But it might be hard to drive to the nearest cardiologist for someone living in a rural area.
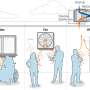
Remotely connecting rural doctors to specialists
For Cobanov's young thyroid patient and her family, technology meant they didn't have to wait for answers, however.
Through an initiative called the MAVEN Project, Dr. Debbie Cohen, a retired pediatric endocrinologist who volunteers her time and expertise, helped make sense of the girl's fluctuating numbers. Cohen determined that the girl went from having hypothyroidism (underactive thyroid) to hyperthyroidism (overactive thyroid).
MAVEN, short for Medical Alumni Volunteer Expert Network, connects expert volunteers across more than 40 clinical specialties with primary care providers serving mostly poor and uninsured patients at more than 90 clinic sites. The volunteers can mentor, participate in patient consultations, and offer provider education.
By bridging gaps in America's health safety net via computers and smartphones, the MAVEN Project aims to "stabilize the frontline primary-care provider workforce in these communities," said Dr. Lisa Bard Levine, CEO of the project.
Copyright © 2020 HealthDay. All rights reserved.