Better planning could save millions in health care costs
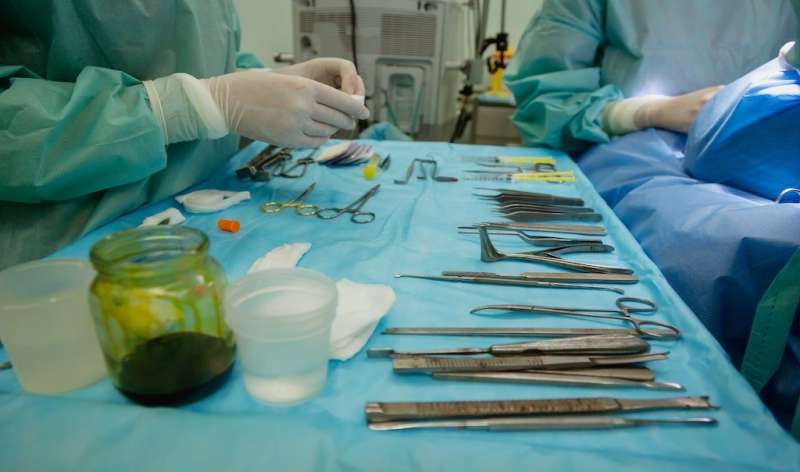
Nearly 30% of the $3.6 trillion spent on health care costs in the United States is wasted. New research from Michigan State University and Rutgers University reveals the amount of money washed away in hospital operating rooms, offering solutions to save hospitals—and the country—millions of dollars each year.
The paper, published in the Journal of Operations Management, found that five to 10 minutes were added to each surgery due to unplanned supplies. Additionally, an average $1,800 per surgery—nearly $28 million annually—could be saved by more frequently planning the supplies needed for a surgery.
"This problem is due to the fact that quality of care has always taken precedence over cost—and rightly so," said Anand Nair, professor of operations and supply chain management and lead author of the study. "However, with increasing pressure on health care organizations, they are trying to find ways to jointly increase quality and reduce costs."
Nair—along with co-authors David Dreyfus, assistant professor at Rutgers Business School and alumnus of MSU's doctoral program, and Claudia Rosales, assistant professor of supply chain management at MSU—found that not only do unplanned costs affect a hospital's bottom line, but they can also endanger patients under anesthesia with potentially harmful complications.
The team spent more than 250 hours observing hospital operating rooms, taking note of processes, preparation and performance of 92 surgeries. Ultimately, they found that the greatest issue stems from a lack of standardization for the planning processes.
"In most hospitals, every surgeon is allowed to make their own decisions in terms of equipment and supplies," Nair said. "Surgeons are comfortable using certain supplies due to their past experiences; this increases the variance among items and the number of items that hospitals need to carry in inventory."
Surgeons request equipment and supplies they need on what's called a physician preference card, or PPC.
With different surgeons requesting preferred equipment for procedures, hospitals end up fulfilling multiple personalized requests, Nair explained. Additionally, without a standardized planning process, teams must address supply shortages during surgery, which can reduce quality, increase costs and present possibilities of potential security lapses.
"If a doctor doesn't have what they immediately need, a surgical team member must find it, which becomes an unplanned cost—and potentially a health risk if they leave the area," Nair said. "On the other hand, if a surgeon requests something that isn't necessary for the surgery, it's simply a waste of money."
Nair explained that some surgeons err on the side of caution and carry supplies in case they might be needed. While this is important given the critical nature of surgeries, a more standardized use of PPCs—along with audits of what supplies are on them—will allow hospitals to reduce redundancies.
Nair explained that minor changes in processes can add up to big savings.
"Managing medical supplies is a critical aspect of the health care supply chain," Nair said.
"Mechanisms need to be put in place to provide more learning opportunities from such operational failures for long-term benefits to happen."
Another complication in hospital rooms is that surgical teams change often, which makes it difficult to communicate which supplies on the PPC aren't consistently used. Open communication among surgical teams helps anticipate needs and reduces unplanned costs in a surgery.
The researchers acknowledge that savings aren't always immediate, but that progress happens along the way during any procedure.
"Our research should encourage hospitals to embrace systems that can better track unplanned costs and plan ahead," Nair said. "Hospitals should explore methods to incentivize surgeons to plan more often. This may be achieved by providing visibility about unplanned costs and workarounds, offering greater control on administering supplies and rewarding for unplanned cost reduction."
More information: David Dreyfus et al, The impact of planning and communication on unplanned costs in surgical episodes of care: Implications for reducing waste in hospital operating rooms, Journal of Operations Management (2019). DOI: 10.1002/joom.1070