Genome analysis has important implications for COVID-19 clinical trials
Scientists at the University of Bristol who have been sequencing the genetic material from SARS-CoV-2—the virus that causes COVID-19—have highlighted important implications for scientists around the world conducting vaccine trials aimed at preventing the disease. The findings are published on the preprint site bioRxiv.
Researchers from Bristol's School of Cellular and Molecular Medicine have been growing the live human SARS-CoV-2 virus in a controlled lab to investigate what the virus is doing inside monkey and human cells.
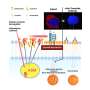
Using state-of-the-art scientific techniques, the team isolated parts of the SARS-CoV-2 virus to find out how the virus instructs the cell to make virus proteins, which can either be used to form virus particles or slow our immune response. The team was also able to investigate whether the genome of the virus changes during growth in cells.
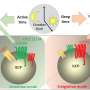
In this paper, the researchers show that when the virus is grown in the laboratory in monkey cells it can make significant changes to the protein found on the surface of the virus—this is called the "spike glycoprotein" which promotes entry into the host cell and is an important target for the human immune system in its fight against the virus.
They also describe that many of the proteins the virus makes are also decorated with important modifications known as phosphorylations which can alter how the virus protein functions and may provide clues about what kinds of drugs might be helpful to treat the virus. There are some drugs, already licenced to treat medical conditions, which act by altering the pattern of phophorylation on proteins. In theory, these drugs might alter the pattern of phosphorylation on virus proteins in an infected person and interfere with virus replication.
Importantly, the findings have implications for scientists conducting vaccine research and those searching for synthetic antibodies to treat infection. Because, when grown on a large scale in the laboratory, the virus might alter the spike glycoprotein. Such a change may mean that when this altered virus is used in important animal clinical trials it might make it harder or impossible to understand if a vaccine or synthetic antibody is working or not.
Dr. Andrew Davidson, Reader in Systems Virology and Dr. David Matthews, Reader in Virology from Bristol's School of Cellular and Molecular Medicine, who have been working on coronaviruses since 2002, explained: "Scientists around the world are working to test vaccines and therapeutic synthetic antibodies against the virus. In order to do that they will need to grow large amounts of virus in the laboratory. They will use this laboratory-grown virus in animal models and work out if their vaccines or therapeutic antibodies actually work and protect animals from the virus.
"Our findings show that when the virus is grown on a large scale it might alter the spike glycoprotein and that teams working on vaccines and drug testing will need to take extra care to make sure the virus is not changing when they grow it up in the lab."
The team, who have been working alongside colleagues from the University of Liverpool and Public Health England (PHE), continued: "Our aim is to help researchers around the world make sure their virus stocks are suitable for their research by investigating how the virus changes in the lab compared to the virus that grows in people."
More information: Andrew D. Davidson et al. Characterisation of the transcriptome and proteome of SARS-CoV-2 using direct RNA sequencing and tandem mass spectrometry reveals evidence for a cell passage induced in-frame deletion in the spike glycoprotein that removes the furin-like cleavage site, bioRxiv (2020). DOI: 10.1101/2020.03.22.002204