COVID-19 evidence and strategies for orthopaedic surgeons
How should orthopaedic surgeons respond to the COVID-19 pandemic? A review in The Journal of Bone & Joint Surgery analyzes evidence and strategies for managing the novel SARS-CoV-2 virus—including critical lessons from past pandemics.
"Controlling the spread of COVID-19 has become the singular focus on several countries, with unprecedented international collaboration and rapid dissemination of emerging scientific evidence," according to the rapid evidence review by Mohit Bhandari, MD, Ph.D., FRCSC, and colleagues of McMaster University, Hamilton, Ont., Canada. In a comprehensive review, they identify and analyze available evidence on the COVID-19 pandemic.
COVID-19—Emerging Evidence and Evolving Strategies
Although the global spread and societal impact of SARS-CoV-2 may seem unprecedented, it is the third major outbreak of coronavirus infection to occur in less than 20 years—following severe acute respiratory syndrome (SARS) in 2002-03 and Middle East Respiratory Syndrome (MERS) in 2012.
Symptoms of COVID-19—most commonly fever and cough—appear an average of five days after infection and almost always within 11.5 days. Evidence suggests that about 20 percent of cases are severe or critical, while about 88 percent have abnormal findings on chest CT scans. Estimates of mortality vary but may approach four percent in confirmed cases of COVID-19. Older patients and those with comorbid conditions, such as cardiovascular disease and diabetes, are at higher risk of death.
There is currently no specific treatment for COVID-19. Trials are underway to evaluate antivirals and other potentially beneficial medications; some of these treatments "may be trialed if available in severe cases." The race is on to develop an effective vaccine against SARS-CoV-2, with several potential targets being evaluated. However, as the authors write, "[A] vaccine that is ready for widespread use is likely still months, possibly years, away."
In the meantime, hygiene, social distancing, and isolation measures are needed to curb virus transmission. Experience suggests that these measures have been effective in "flattening the curve" of viral transmission—as demonstrated by the textbook example of the 1918 influenza pandemic. In that historic epidemic as in the SARS pandemic, a second wave of infections occurred after relaxation of containment measures.
"It is essential that we continue these practices, as the outbreak is currently expected to last for many more months and we must be mindful of the lessons learned from past pandemics to prevent a second wave from occurring," according to Dr. Bhandari and colleagues. That's especially important in limiting the spread of SARS-Cov-2 by asymptomatic and pre-symptomatic individuals.
Guiding Surgeons Through the Pandemic
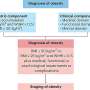
The authors summarize recent guidance to surgeons and other frontline healthcare professionals, including postponing or cancelling elective or nonemergency surgical procedures; shifting inpatient tests or procedures to outpatient settings, if possible; and taking steps to conserve available resources and healthcare capacity. The review includes recommended steps for necessary surgery in patients with COVID-19.
Dr. Bhandari is Editor-in-Chief of OrthoEvidence, a global online source for high quality and timely orthopedic-only, evidence-based summaries. In partnership with JBJS, OrthoEvidence has created a COVID-19 Resource Center, offering podcasts, original content, links to critical breaking studies, and global perspectives on COVID-19 from orthopaedic surgeons around the world on how they're responding to the pandemic.
"Data is the differentiator in this global crisis," Dr. Bhandari writes in a message to the OrthoEvidence community. "We are proud to stand with our community to provide as much evidence as we can to help you all make important decisions for your communities and your patients."
Click here to read "Novel Coronavirus COVID-19: Current Evidence and Evolving Strategies."DOI: 10.2106/JBJS.20.00396
More information: Christopher Vannabouathong et al. Novel Coronavirus COVID-19, The Journal of Bone and Joint Surgery (2020). DOI: 10.2106/JBJS.20.00396