A near-infrared light treatment could help manage a rare form of lung cancer
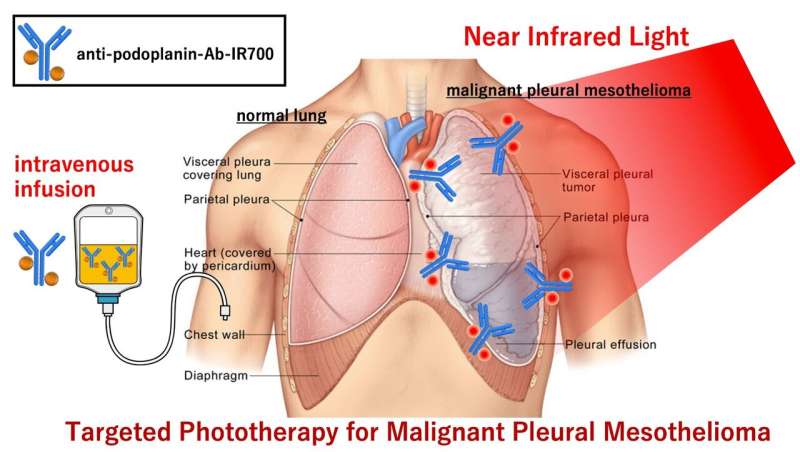
Treating a rare type of malignant lung cancer could improve, thanks to near-infrared irradiation and a cancer-targeting compound. Nagoya University oncologist Kazuhide Sato and colleagues tested the treatment and published their findings in the journal Cells.
Malignant pleural mesothelioma (MPM) is a rare type of cancer that affects the lung lining. It rarely spreads to other parts of the body, but is usually diagnosed too late, leading to a poor prognosis and very limited treatment options.
Sato and colleagues investigated the effectiveness of near-infrared photoimmunotherapy (NIR-PIT) as a treatment strategy for MPM. NIR-PIT has been fast-tracked for approval by the U.S. Food & Drug Administration for treatment of a type of malignant head and neck tumor. For NIR-PIT to work, a cancer-targeting compound must first be injected. The compound is made of an antibody, which targets a specific structure on the cancer cells, and a photoabsorber, called IR700. When near-infrared light is shone on the body part affected by cancer, the compound aggregates on the cancer cell membranes, leading to acute cell rupture and tumor death.
"The lungs and chest cavity contain a large amount of air and are thus very good at effectively transmitting near-infrared light," says Sato. "NIR-PIT is a safe phototherapy option that can target a region of interest. The antibody-IR700 conjugate is also non-toxic to the body in the absence of near-infrared light irradiation. We thus thought that NIR-PIT could be an effective strategy for controlling localized MPM."
For NIR-PIT to work on MPM, the scientists needed a compound that specifically targeted MPM cancer cells. They focused their attention on an antibody called NZ-1, which targets a specific part of a transmembrane glycoprotein called podoplanin. Podoplanin is normally found on many cell types in the human body, but is particularly abundant in some types of cancer cells, including MPM.
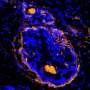
The team's research showed that podoplanin was widely expressed in a variety of MPM cell lines. They found that NZ-1 conjugates well with the photoabsorber IR700 and that NZ-1-IR700 specifically bound to podoplanin on cells in the lab. When podoplanin-positive cells, including MPM cancer cells, were mixed with NZ-1-IR700 and then irradiated with near-infrared light, the cells immediately swelled and ruptured.
The team then injected NZ-1-IR700 in mice with MPM tumors. The compound gradually accumulated at the tumor sites. Shining near-infrared light on the tumor sites led to a reduction of fluorescence from cancer-tagged cells, indicating the treatment worked well as an anti-cancer strategy.
Sato and his colleagues say further studies are needed to find ways that ensure the treatment will not kill healthy podoplanin-positive cells. The researchers also suggest a more focused dose of light could be achieved by shining it into a drainage device inserted into the chest cavity, which is normally used anyway in MPM patients to drain the chest from excess fluids.
More information: Yuko Nishinaga et al. Targeted Phototherapy for Malignant Pleural Mesothelioma: Near-Infrared Photoimmunotherapy Targeting Podoplanin, Cells (2020). DOI: 10.3390/cells9041019