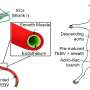
New 3-D-printed artery can monitor blockages from the inside

When surgeons replace part of a blood vessel—something they do in 450,000 patients per year in the United States to treat blood clots, coronary disease, stroke damage and more—the grafted vessel is monitored by CT scans, ultrasounds and other expensive imaging techniques. Despite all that effort, between 40% and 50% of those grafts fail.
That's one reason University of Wisconsin–Madison materials science engineers are developing a new, 3-D-printed artificial blood vessel that allows doctors and patients to keep tabs on its health remotely.
The implantable vessel, made of a flexible composite and capable of real-time monitoring, is described in a new study published in the journal Advanced Functional Materials by UW–Madison professor Xudong Wang and graduate student Jun Li.
"This artificial vessel can produce electric pulses based on pressure fluctuation which will be able to tell precisely the blood pressure in the vessel without using any additional power source," says Wang. "And because of the 3-D geometry, the electric pulse profile will be able to tell if there is an irregular motion due to blockage inside in the very early stages."
The artery project stems from Wang's long-term research interest in new soft, flexible materials that are piezoelectric (able to produce an electric charge from mechanical stress) and biocompatible (able to be used in the human body without causing rejection or damage).
The team combined sodium potassium niobite piezoceramic nanoparticles with a polyvinylidene fluoride polymer which is ferroelectric, or able to flip polarity when an electric field is applied. They then printed a tubular artery using the material and an off-the-shelf 3-D printer. The printer extrudes the material through a strong electric field close to the nozzle to polarize the ceramic particles, giving the structure its piezoelectric property.
Li put the artificial artery through its paces, hooking it up to an artificial heart system before simulating blockages, high blood pressure and other issues that face artificial blood vessels. The self-powered material was able to correctly detect changes in force and pressure within the artery.
The researchers' next step is to optimize the production of the new ferroelectric composite and the 3-D printing process. The team also wants to find ways to make the printed 3-D structure even more sensitive, and plans to collaborate with researchers in the biomedical field to test the artery with even more realistic models of the circulatory system.
Additionally, they hope to use the new material to print artificial heart valves. Replacement heart valves are typically either mechanical or taken from human or animal donors, and none incorporate the type of self-monitoring found in Wang's material. The team, which includes collaborators from UW–Madison's School of Medicine and Public Health and Zhejiang University in China, believes that in the future it may be possible to use the ferroelectric biomaterial and 3-D printer to create other custom, artificial organs.
While researchers are working on many other types of artificial blood vessels and organs, Wang thinks this technique has some advantages over more complicated techniques.
"This is an easy, scalable technology," he says. "Our new printable composite material allows us to make a 3-D structure in one step that can show multi-functionality right out of manufacture."
More information: Jun Li et al. Multifunctional Artificial Artery from Direct 3D Printing with Built‐In Ferroelectricity and Tissue‐Matching Modulus for Real‐Time Sensing and Occlusion Monitoring, Advanced Functional Materials (2020). DOI: 10.1002/adfm.202002868