Type III interferon in COVID-19: Protective or harmful?

Our immune system makes interferons and other cytokines to help us fight viruses. But in COVID-19, we've learned that they can also contribute to damaging, potentially life-threatening lung inflammation. New work published yesterday in the journal Science helps tease out the good from the bad for one interferon of interest: type III.
Recent evidence suggests that type III interferon, a.k.a. interferon lambda (λ), can fight viral infection while also limiting inflammatory damage. That has led to at least two clinical trials to test them as a treatment for COVID-19.
But the new study raises a caveat. Researchers at Boston Children's Hospital, with collaborators in Italy, provide evidence that type III interferon increases the risk of life-threatening bacterial "superinfections" in the lung. These superinfections can happen in both influenza and COVID-19. The investigators caution that type III interferons given later in the course of COVID-19 could do more harm than good.
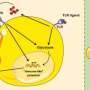
"Our data indicate that the new coronavirus, SARS-CoV-2, inhibits interferon production in the upper airways," says Ivan Zanoni, Ph.D., an immunologist at Boston Children's and the study's senior investigator. "This weakens the immune response and helps the virus survive. But when the virus reaches the lower airways, there is an exuberant immune response, including an increase in type III interferons that we think is harmful."
Interferon in COVID-19: Location, timing are key
The team first tested samples from patients with severe COVID-19 and healthy controls. Interferon III was not much increased in the patients' nasopharyngeal swab samples. But it was markedly elevated in their lung fluid.
Next, the researchers exposed mice to synthetic viral RNA to mimic the effects of SARS-CoV-2 infection in the lower airways. Interferon III levels rose markedly in the animals' lungs as compared with control mice. Continued production of interferon III prevented the lungs from maintaining their protective surface barrier.
This, in turn, made the mice more susceptible to lethal bacterial infections from Staphylococcus aureus. Experiments showed increased amounts of bacteria in the lungs and higher mortality as compared with control mice.
"There's still a lot to understand, but it looks like location and timing of interferon production are key," says Zanoni. "Early during SARS-CoV-2 infection, when the virus is in the upper airways, it might be important to intervene with recombinant interferons and other antivirals. But later on, when inflammation increases in the lower airways, it will be important to block the signaling cascade initiated by interferons and other inflammatory cytokines, possibly with the anti-inflammatory drugs."