Aggregated waste in brain tumors predict disease severity
Proteins are crucial to all cellular processes. So for a cell to stay viable, it has to keep its proteins in shape. In technical terms, it's called protein folding, and it refers to the process by which proteins assume their biologically functional 3-D structure. Proteins can quickly misfold under elevated stress or heat, and misfolded proteins lose their functionality and even clump into harmful aggregates.
Therefore, proteins are constantly surveyed by a protein quality control system, or PQC. The PQC can fold, refold, or if necessary, terminally degrade misfolded proteins. However, the protein quality machinery can be overwhelmed, forcing the cell to triage toxic protein waste into a garbage bin-like structure called the aggresome, which acts as a PQC last line of defense and is eventually cleared when cellular stress is alleviated.
"Cancer cells are no different. As they are highly active and rapidly dividing, they need to keep the toxic waste under control," says Dr. Shahenda El-Naggar, director of the Research Department at the Children's Cancer Hospital Egypt (CCHE) 57357.
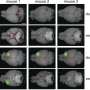
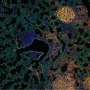
El-Naggar is the corresponding author on a recent manuscript published in the Journal of Neuro-Oncology reporting altered PQC activity in choroid plexus tumors (CPTs), which is a rare pediatric brain tumor. After examining 42 CPT tissues archived at the CCHE Pathology Department, her team has successfully identified a correlation between the percentage of tumor cells containing aggresomes and disease severity. They report tumors having more than 25% aggresome-positive cells being the most aggressive, which may affect the treatment decision.
Traditionally, CPTs are classified into three subgroups according to their histological features (how they look under the microscope), while advanced molecular classification divides this type of tumor into two distinct subgroups. Interestingly, all of the aggressive histological and molecular subgroups contained aggresomes.
In a previous study, the team also used aggresomes to predict the prognosis of medulloblastoma, another aggressive pediatric brain cancer. Therefore, the results validate the efficiency of aggresomes as a molecular prognostic tool for two aggressive pediatric brain tumor types. In the current study, the team decided to further investigate the altered pathways in the aggresome-positive CPTs.
"Unraveling the main altered pathways in CPTs could deepen our understating of the disease pathogenesis; it might also uncover novel therapeutic targets," said Nada Amer, the first author on the paper.
The team extracted the whole genetic material (genome) and whole expressed proteins from the tumors' tissues. Then, they performed a technique called whole-genome DNA methylation analysis that could offer a glimpse into the altered pathways between benign and malignant tumors.
DNA methylation is a normal biological process that orchestrates the activity of our genes by adding methyl groups at certain critical locations and switching off some genes. Any abnormal alteration of the methylation pattern disrupts the fine-tuned genomic orchestra.
The analysis revealed altered methylation signature in several genes associated with PQC activity in the aggresome-positive and the aggressive molecular type. This was also evident when the team compared the differentially expressed proteins between the distinct subgroups.
"One of the most interesting findings was the hypermethylation of members of the ZIC family of transcription factors in critical locations," Amer says. She explains that those genes are crucial to the normal development of brain cells, and they were reported to be silenced in other types of aggressive tumors. "Overall, our data support that aggresomes are not only a valuable prognostic marker, but might also offer a potential target for CPT treatment in the future," El-Naggar says.
More information: Nada Amer et al. Aggresomes predict poor outcomes and implicate proteostasis in the pathogenesis of pediatric choroid plexus tumors, Journal of Neuro-Oncology (2021). DOI: 10.1007/s11060-020-03694-3