Model helps predict which patients will benefit most from PSMA PET scan

A new study led by researchers at the UCLA Jonsson Comprehensive Cancer Center helps identify which patients with prostate cancer will benefit most from the use of prostate-specific membrane antigen PET imaging, PSMA PET, a novel imaging technique that recently was approved by the U.S. Food and Drug Administration.
By studying different variables and risk factors, researchers created a model that can be used in the clinic to identify patients who may have more extensive disease than anticipated and identify patients who are at higher risk of prostate cancer spreading to lymph nodes in the pelvis and beyond. The team found the percent of positive cores—a metric that reflects volume of disease—is a powerful predictor of increased nodal, metastatic and any upstaging in men with newly diagnosed high-risk prostate cancer. Patients with PPC greater than 50% and had a Gleason score of 9 or 10 (Gleason grade group 5) are the most likely to benefit from getting the PSMA PET scan.
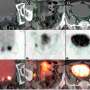
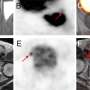
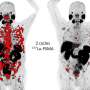
The PSMA PET scan is an emerging imaging modality with improved sensitivity and specificity over conventional imaging for prostate cancer staging. It uses positron emission tomography (PET) in conjunction with a tracer that is highly effective in detecting prostate cancer throughout the body so the precise location of the full extent of disease can be visualized. The PSMA PET scan identifies cancer that is often missed by current standard-of-care imaging techniques. However, this scan is still not widely available and resource allocation may be a problem. Therefore, it is imperative to identify patients who are most likely to benefit from this novel imaging technique.
The team looked at 213 men who were enrolled in two prospective clinical trials at UCLA that used the PSMA PET scan as a part of primary staging of the disease. They used a multivariable logistic regression model to assess for predictors of upstaging and developed a risk calculator to further quantify the risk for each individual patient.
The findings could help predict which patients may have more cancer than anticipated, spreading to pelvic lymph nodes and beyond. An easy-to-use nomogram (calculator) was also developed as part of the effort. This is crucial for designing optimal treatment plans for each individual patient.
More information: Amar U. Kishan et al, Identifying the Best Candidates for Prostate-specific Membrane Antigen Positron Emission Tomography/Computed Tomography as the Primary Staging Approach Among Men with High-risk Prostate Cancer and Negative Conventional Imaging, European Urology Oncology, 2021, ISSN 2588-9311, DOI: 10.1016/j.euo.2021.01.006