Fecal microbiota transplantation for active peripheral psoriatic arthritis shows no advantage
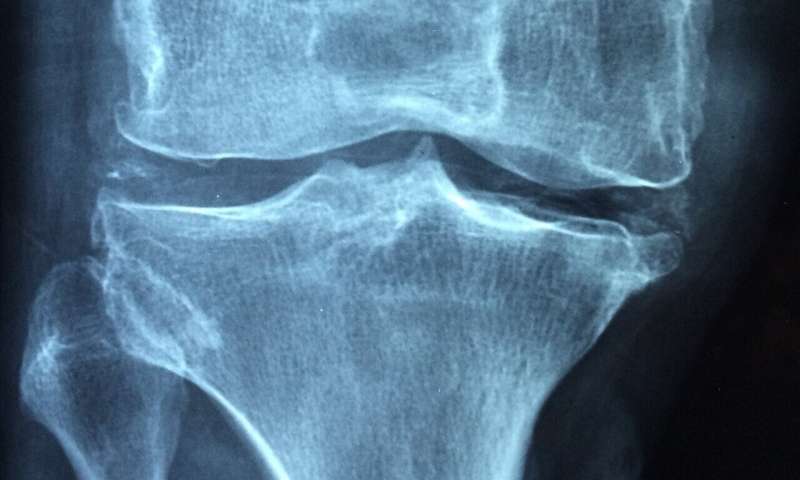
In this proof-of-concept study, Maja Skov Kragsnaes and colleagues evaluated efficacy and safety of FMT in people with psoriatic arthritis (PsA). PsA is an inflammatory arthritis that causes a person's joints to become stiff and painful. It is often found people with the skin condition psoriasis, and there is also a link between PsA and inflammatory bowel disease or gastrointestinal symptoms.
This double-blind, parallel-group, sham-controlled, superiority trial randomly allocated 31 adults with active peripheral PsAd despite ongoing treatment with methotrexate to one gastroscopic-guided FMT procedure, or sham transplantation into the duodenum. The transplants (50 g feces) came from one of four healthy, anonymous stool donors. The primary efficacy endpoint was the proportion of participants experiencing treatment failure, defined as needing treatment intensification through 26 weeks, and safety was monitored throughout.
The results showed that treatment failure occurred more frequently in the FMT group than in the sham group (60% versus 19%, and improvement in function was also in favor of sham. No serious adverse events were observed.
More information: Kragsnaes MS, et al. Efficacy and safety of faecal microbiota transplantation for active peripheral psoriatic arthritis: a randomised sham-controlled trial. Presented at EULAR 2021. Abstract OP0010.