Existing leukemia treatment could hold promise for Bile duct cancer
Bile duct cancer is a rare but aggressive form of cancer, affecting just over 2,000 people in the UK every year. However, incidences of bile cancer are steadily increasing every year—with some estimating it could one day be as common as breast cancer.
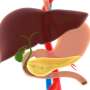
Also known as cholangiocarcinoma, bile duct cancer happens when the lining cells of the biliary ducts (a network of tubes that connects the liver, gallbladder, and small intestines) grow out of control and accumulate in the ducts, subsequently blocking drainage of bile from the liver. Genetics, molecular changes (such as protein modifications) and environmental factors (such as exposure to chemical compounds like nitrosamines, arsenic) are all possible causes.
But it's often difficult to diagnose bile duct cancer because there are few symptoms—and the most common early symptom, jaundice (yellowing of the skin, whites of the eyes and mucous membranes), may be mistaken for other, more manageable diseases, such as gallstones or hepatitis. Early tumors are also rarely detectable during routine examinations because the bile ducts are located deep inside the body.
Because of this, by the time bile duct cancer is diagnosed it's often too late. The five-year survival rate for patients with the disease is between 5-30%, depending on how early the cancer is diagnosed, and whether the tumor is inside or outside the liver. Deaths from bile duct cancer have also been steadily increasing in the last two decades.
What's more, patients have very limited treatment options. The only realistic way to cure bile duct cancer is surgically removing the tumor—when operable. But our latest research may have found a way to treat bile duct cancer using cancer treatments that already exist.
Recent discoveries
In the last decade, researchers have focused on targeting specific genes and proteins involved in the growth and survival of cancer cells to better understand this type of tumor. This has seen the development of a plethora of new drugs, some of which are already helping to improve outcomes for certain patients. But there are still no cures available.
In a major new study published in Hepatology our research group proposes that the drug all-trans retinoic acid (ATRA) could be used to help treat bile duct cancer.
ATRA is the active metabolite (small molecule) of vitamin A. ATRA is involved in cell differentiation (where one cell turns into a specific type of cell), and cell death. It's also used to treat certain types of blood cancers—such as acute promyelocytic leukemia. Although using ATRA to treat this type of leukemia is well established and tolerated in patients, research on its use in solid tumors is limited.
Using mouse models, our research showed that ATRA shrinks tumors by 40% compared to a placebo treatment. ATRA works to reduce the incidence of tumors through specific molecules—such as nuclear retinoic acid receptors, a type of receptor that controls the presence or absence of certain proteins. More recently, it's been shown that ATRA suppresses the expression and activation of a protein called PIN1, a master regulator of cancer-causing genes and tumor suppressors in tumor cells.
Our team showed that PIN1 is abundant in liver biopsies of patients with bile duct tumors. ATRA works to reduce the abundance of PIN1 in cells and animal models of bile duct cancer.
The best news is that ATRA's effects on PIN1 has no negative impact on the nearby healthy cells lining the bile ducts. This shows us both the function of PIN1 in causing tumors—and the specific anti-tumoural effect of ATRA. We also discovered that a protein, called JNK, is responsible for allowing PIN1 to remain stable and accumulate in cancer cells—ultimately advancing tumor growth.
Research is ongoing to understand whether inhibiting PIN1 with ATRA (or other similar therapies) could work together with current bile cancer therapies (such as cisplatin or gemcitabine). Human trials will also need to be conducted.
But given ATRA is safe, well-tolerated, and its use is being tested in clinical trials of breast and pancreatic cancers, we hope our findings could quickly progress into clinical trials for bile duct cancer in the future.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()