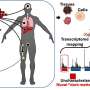
Researchers use gene editing to tackle facioscapulohumeral muscular dystrophy
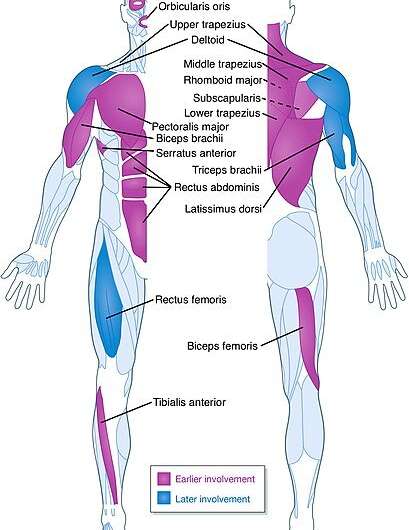
Roughly 1 out of 15,000 people born suffer from Facioscapulohumeral Muscular Dystrophy (FSHD), a rare disease that starts with the progressive weakening of facial muscles and then the shoulders and upper body. By the time patients reach their 50s, around one-fifth of them are wheelchair bound.
Now, a team of Florida State University researchers has found that using sophisticated gene-editing techniques, they can essentially turn off or remove part of the genetic code that leads to the disease— a move that opens the door for potential therapies to reverse or stop progression of the disease.
The work is published in Scientific Reports.
"Applying genome engineering to excise the pathogenic element in FSHD was enormously challenging due to the repetitive nature of the chromosomal region responsible for the disease, but I was delighted to be able to obtain the result we were hoping for," said former FSU graduate student Sunny Das, the lead author of the study. "My hope is that these results will open the door to the very real potential of a new therapeutic possibility."
FSHD is a complicated genetic disease with no known cure. In the mid-1990s, scientists discovered it was associated with chromosome four, which is responsible for a little more than 6 percent of DNA in human cells. The end of that chromosome has a DNA sequence that can repeat dozens of times—an average person might have 100 copies or more, but a person with FSHD typically has less than 10 copies.
Within these repetitive sequences is a gene called DUX4, which plays a major role in the early embryonic stages of human development and then gets turned off in adult tissues. However, if it somehow turns back on, humans can develop FSHD.
"It's an incredibly complex genetic disease," said Associate Professor of Biological Science Brian Chadwick, a co-author on the study and Das' graduate adviser. "But what we do know is the inappropriate expression of DUX4 is driving the atrophy of muscles in individuals."
Chadwick and Das, who is now a postdoctoral researcher at Massachusetts Institute of Technology, acquired patient muscle cells to see if they could potentially use genetic tools to repress the disease in some way.
They divided the cell lines into two separate experiments. For one experiment, they used CRISPR to essentially cut out the small element of DNA that normally would allow DUX4 to activate, thus preventing it from being turned on. For the second, they used biochemical tools to see if they could basically turn off DUX4 expression without deleting the underlying genetic sequence.
Both methods worked.
Chadwick noted that several other research groups around the globe have also published similar results over the past few months.
"What that means is this kind of prioritizes further development of therapies where you can go in and engineer out this element in patient cells to see if you can stop the progression of the disease or reverse it," he said.
More information: Sunny Das et al, CRISPR mediated targeting of DUX4 distal regulatory element represses DUX4 target genes dysregulated in Facioscapulohumeral muscular dystrophy, Scientific Reports (2021). DOI: 10.1038/s41598-021-92096-0