Low BMI and malnutrition, but not obesity, are risk factors for older adults dying from COVID-19
A recent study published in Clinical Nutrition shows that low BMI and malnutrition are risk factors for in-hospital mortality in geriatric COVID-19 patients. The study was performed at Karolinska Institutet in collaboration with Theme Inflammation & Aging at Karolinska University Hospital and geriatric clinics in the Stockholm Region.
These results are important as information on the groups with the highest mortality, i.e. the very old and frail patients, is underrepresented. For example, obesity is a risk factor in COVID-19 infection in younger adults but we instead found that low BMI and malnutrition increased the risk of in-hospital mortality in geriatric COVID-19 patients who were mostly older than 75 years, says Ph.D. Laura Kananen, a researcher at the Department of medical epidemiology and biostatistics, KI.
COVID-19 in hospitalized geriatric patients
During the first COVID-19 wave in the spring 2020 in Sweden, researchers at Karolinska Institutet reported that in-hospital mortality was 24% among older hospitalized geriatric patients. The risk of death was almost doubled for patients classified as frail according to the Clinical Frailty Scale (CFS) as compared to non-frail older patients. In these patients, acute kidney injury and multimorbidity were also strong risk factors for death.
BMI and nutritional status as risk factors?
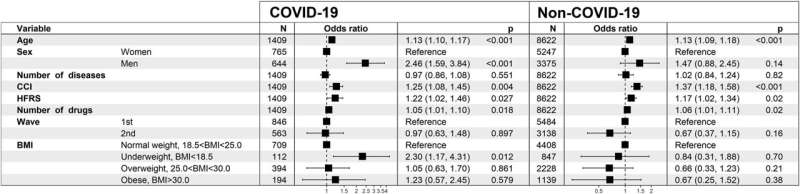
The role of body composition and nutritional status in COVID-19 pathology has not been characterized well in hospitalized older adults (>65 years). Therefore, in our study, we analyzed the associations of body mass index, and nutritional status assessed using Mini Nutritional Assessment-Short Form (MNA-SF) with in-geriatric hospital mortality in older patients treated for COVID-19. As a reference, the analyses were performed also in older patients who were hospitalized for other causes than COVID-19 in the same geriatric hospitals during the same time period. Data in the analysis comprised medical records of ~10 000 patients in Stockholm during the first two pandemic waves. Age range of the patients was from 65 to 105 years, and their median age was 83 years. Follow-up of survival was short, i.e., only the hospitalization period.
The major finding of this study was that indicators of undernutrition; i.e., underweight (BMI<18.5) and low MNA-SF scores (0–7), were related to short-term mortality in the COVID-19 patients. MNA-SF predicted death also in patients who were hospitalized for other causes. No evidence was found that obesity is a risk factor in COVID-19 infection in the older patients. While the capacity of MNA-SF as a prognostic factor has been shown earlier beyond COVID-19, i.e., it predicts short-and long-term mortality, our finding is a reminder that nutritional status is vital to examine and to treat in geriatric patients. Our study offers evidence-based guidance for the clinical work with geriatric patients.
More information: L. Kananen et al, Body mass index and Mini Nutritional Assessment-Short Form as predictors of in-geriatric hospital mortality in older adults with COVID-19, Clinical Nutrition (2021). DOI: 10.1016/j.clnu.2021.07.025