Advances in sleep disorder diagnostics: Simpler measurements, more accurate analyses

Sleep disorders and insufficient sleep are major global problems contributing to, e.g., increased health care costs and sick leaves, and reduced quality of life. According to recent estimates, sleep apnea alone affects approximately 1 billion people worldwide, and up to half of the world's population suffers from insomnia at some point in their lives. In Finland alone, sleep apnea is estimated to affect the lives of nearly 1.5 million people despite most of them remaining undiagnosed. Simpler and more cost-effective methods for screening and diagnosing sleep disorders are urgently needed.
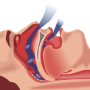
A recent review by the Sleep Technology and Analytics Research group, STAR, at the University of Eastern Finland examined future trends in sleep disorder measurement technology, focusing on the possibilities of at-home measurements. Polysomnography, currently performed in sleep laboratories in specialized health care, is the most comprehensive method for diagnosing sleep disorders. However, due to the high price and limited availability of in-laboratory polysomnography, other methods, such as simple self-applied home sleep recordings, are also used in the diagnosis of sleep apnea. Technological advances in measurement technology, as well as in analysis methods based on machine learning and artificial intelligence, enable the use of simpler and more affordable measurements in hospital settings without compromising clinical accuracy. In research, a number of automated methods to analyze sleep recordings have been developed, and their introduction to clinical practice could free up health care resources. In addition, simpler sensors could enable multi-night sleep recordings, thus providing a more accurate picture of the natural structure of sleep. Although self-applied home sleep recordings cannot fully replace comprehensive polysomnography performed in a sleep laboratory, their use will certainly increase in the future.
With the current technology used in self-applied home sleep recordings, it is challenging to determine the exact structure of sleep. Traditionally, sleep stages are identified based on electroencephalogram (EEG). However, EEG is usually not included in self-applied home sleep recordings as current clinical electrodes require extensive skin preparation before they can be applied, as well as accurate placement in different areas of the head.
A recent study by the STAR group examined the electrical properties of novel textile-based dry electrodes and the quality of the EEG signal captured by them. The study showed that dry electrodes require a longer period to form stabilized electrode-skin contact than silver/silver chloride electrodes, which are widely used in clinical practice. However, in measurements performed in laboratory settings, the EEG signal captured by textile electrodes was found to correspond well to the quality of the signal captured by clinical electrodes.
"Textile electrodes are considerably easier to use and more patient-friendly, and thus a viable alternative to be used in self-applied home sleep recordings," Early Stage Researcher, lead author Matias Rusanen, from the University of Eastern Finland says.
Better-quality at-home measurement methods may also be useful for monitoring of the progression of sleep apnea, as the severity of the disease typically develops over several years. Breathing cessations in sleep apnea usually lead to transient drops in blood oxygen saturation, which puts a significant strain on the patient's body at night. This so-called hypoxic load has also been found to predispose patients to many other diseases, such as diabetes and cardiovascular disease.
Another recent study by the STAR group examined the reverse causality of how existing diseases affect the development of the hypoxic load over several years. The study showed that in patients with diabetes or cardiovascular disease, the worsening of nocturnal hypoxic load was significantly greater during a five-year follow-up than in patients without comorbidities typically associated with sleep apnea.
"Our findings suggest that patients with diabetes or cardiovascular disease could benefit from the screening, and especially continuous monitoring of sleep apnea, and thus from the necessary treatment," Early Stage Researcher, lead author Tuomas Karhu from the University of Eastern Finland says.
Since comprehensive polysomnography is an expensive and complex measurement, it is not very well suited for continuous monitoring. One solution to this problem could be the methods presented above, in which the patient's sleep is monitored by self-applied and reusable sensors in the home environment.
More information: Henri Korkalainen et al, Self-Applied Home Sleep Recordings, Sleep Medicine Clinics (2021). DOI: 10.1016/j.jsmc.2021.07.003
Matias Rusanen et al, An In-Laboratory Comparison of FocusBand EEG Device and Textile Electrodes Against a Medical-Grade System and Wet Gel Electrodes, IEEE Access (2021). DOI: 10.1109/access.2021.3113049
Tuomas Karhu et al, Diabetes and cardiovascular diseases are associated with the worsening of intermittent hypoxaemia, Journal of Sleep Research (2021). DOI: 10.1111/jsr.13441