Could long-dead bacteria be the culprit behind lingering Lyme symptoms?
Even after antibiotic treatment, some Lyme disease patients suffer from an array of symptoms including neurological issues that greatly diminish their quality of life. Brain scans of these patients show persistent neuroinflammation, but the cause has been unclear.
Tulane University researchers have discovered that remnants of B. burgdorferi, the bacteria that causes Lyme disease, may contribute to inflammation in both the central and peripheral nervous systems. These remnants are significantly more inflammatory than live, intact bacteria published in Scientific Reports.
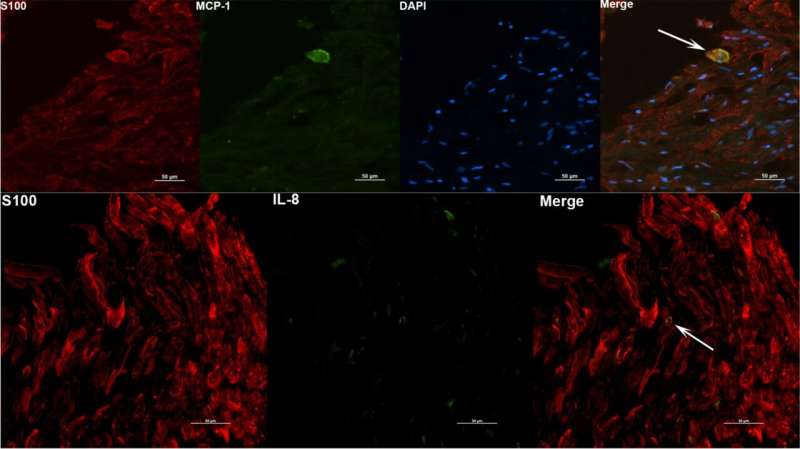
Lead researcher Geetha Parthasarathy, Ph.D., assistant professor of immunology at the Tulane National Primate Research Center, explored the effects of B. burgdorferi remnants on nervous system tissue using a nonhuman primate model, investigating the effects on both the frontal cortex and dorsal root ganglion.
Inflammatory markers in these areas were several times higher in samples exposed to remnants of B. burgdorferi than in samples exposed to live bacteria, and several times higher in the frontal cortex than the dorsal root ganglion. The bacterial remnants also caused cell death in brain neurons.
"As neuroinflammation is the basis of many neurological disorders, lingering inflammation in the brain due to these unresolved fragments could cause long term health consequences," Parthasarathy said.
Scientists still don't know how B. burgdorferi spirochetes find their way into brain tissue. In longstanding or persistent Lyme disease infections, bacterial spirochetes may harbor inside major organs including the heart and brain, where they could continue to wreak havoc over time. Antibiotics may kill the bacteria in these organs, but remnants could remain if the body cannot adequately eliminate them.
Parthasarathy said the findings may explain some of the neurological symptoms and conditions that patients with persistent Lyme infections can experience. She plans future studies to investigate new anti-inflammatory therapies for antibiotic-resistant neuroinflammation and to explore why the body may not be clearing these bacterial remnants.
More information: Geetha Parthasarathy et al, Neuropathogenicity of non-viable Borrelia burgdorferi ex vivo, Scientific Reports (2022). DOI: 10.1038/s41598-021-03837-0

















