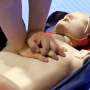
Requiring CPR and defibrillator training in schools can improve survival rates when bystander CPR occurs
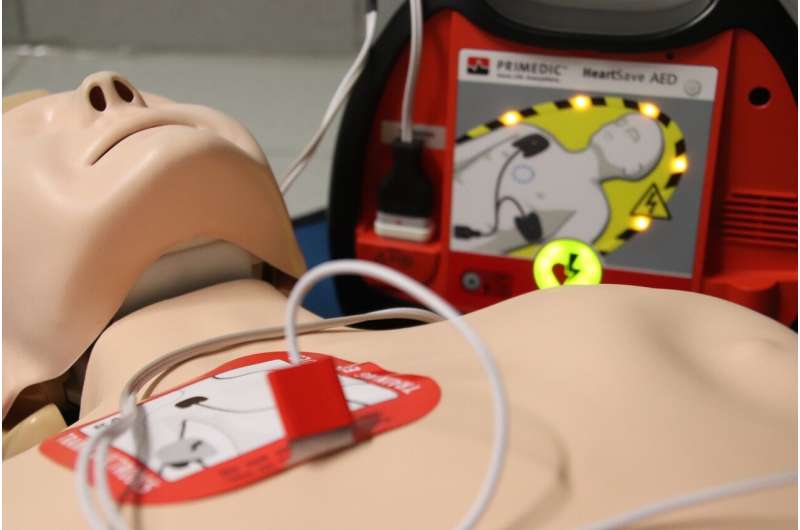
States with laws requiring CPR/automated external defibrillator (AED) training in high school have higher rates of bystander CPR (BCPR) after out-of-hospital cardiac arrest (OHCA) than states with no CPR education laws, according to a study today in the Journal of the American College of Cardiology.
About 377,000 adults and 23,000 children experience an out-of-hospital cardiac arrest (OHCA) each year in the United States, with relatively low survival rates. Reports show that early use of CPR and defibrillation by a trained bystander contribute to lower mortality rates. Many states have enacted required CPR/AED training, specifically in high schools, in anticipation of improving OHCA outcome survival.
"BCPR and AED use rates remain low in the US. Lack of knowledge of CPR and AED use results in failure to perform these life-saving skills when needed," said Victoria Vetter, MD, MPH, an attending cardiologist and cardiac electrophysiologist in the Division of Cardiology at Children's Hospital of Philadelphia and the study's lead author.
In this study, researchers examined whether rates of BCPR following OHCA differ in states with laws requiring CPR/AED training in schools compared to those without such mandates. At the time of the study, CPR/AED training for high school students was required in 39 out of 50 states and the District of Columbia to improve bystander involvement in OHCA events. The study authors analyzed the Cardiac Arrest Registry to Enhance Survival (CARES) dataset from January 1, 2013, through December 31, 2020, for all 911-activated non-traumatic OHCA events where CPR or AED use was attempted. Arrests in medical facilities, nursing homes or those witnessed by 911 responders were excluded.
Twenty states were eligible for evaluation and placed in two separate categories: states with CPR/AED education laws and states without a CPR/AED education law. Cardiac arrests were categorized in states with laws as occurring either on or after the law was enacted (pre- and post-law enactment).
Over half of the OHCAs occurred in states with laws enacted and the rate of BCPR was 41.6%, compared to 39.5% in states without any mandates. After tracking pre- and post-law enactment outcomes by year, rates of BCPR show a higher trend after the first year of state law enactment, specifically in five of the 10 states that had laws enacted during the study period. Researchers found disparities by gender and race in study, but those groups, specifically Blacks, showed the greatest improvements in outcomes in states with laws enacted.
Researchers said the findings also suggest that low economic status communities could see the greatest benefits from help in enacting CPR/AED education mandates.
"Targeting student populations in underserved and minority communities with low rates of BCPR should help by providing a trained group of individuals who live in the communities, decreasing these health disparities," Vetter said. "High school students will become the next generation of bystanders who can provide CPR and AED use, once they are educated. Those trained as students are likely to be in homes or community sites where cardiac arrests commonly occur."
While the study's models accounted for various factors that may influence BCPR rates, limitations include the recent implementation of some BCPR laws. Also, states were not identifiable, so researchers were not able to gather state level characteristics, such as population health measures, which may impact the propensity for laws to be enacted and OHCA outcomes. CARES also does not collect data from all EMS systems, which may limit the true generalizability of the findings.
The study authors said they encourage future research with complete state-specific data and recent implementation of legislation mandates is needed to further support adding CPR education training in schools to improve OHCA survival rates.
More information: Impact of State Laws: CPR Education in High Schools, Journal of the American College of Cardiology (2022).