Study explores how active parent participation can improve neonatal health and reduce parental stress
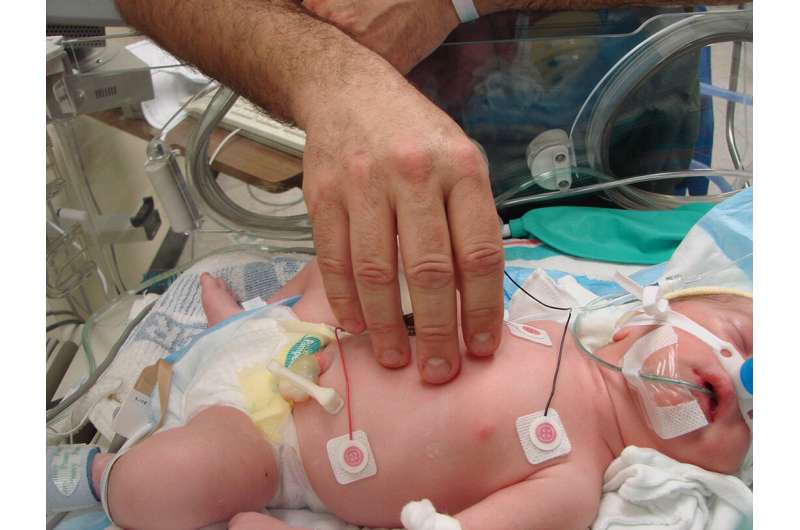
The parent-offspring bond is a fundamental connection for humans. In neonatal care, particularly when caring for ill or preterm infants, special importance is given to active physical closeness between the parents and the infant. Research has shown that preterm infants who receive parental care in the form of physical and emotional closeness have better rates of growth and development. What's more, skin-to-skin contact with infants also reduces parental anxiety and stress. This concept of zero-separation in neonatal care has led to the development of the family integrated care model, where parents are mentored and trained to become the primary caregivers to their infant.
Despite the clear advantages of infant-parent closeness, there is no data available on the current set-up of NICUs in Europe regarding zero-separation. The policies around zero-separation revolve around two basic requirements—the first is the infrastructure and policies in the NICU that support parental participation in neonatal units, like the availability of bed-units, or the hospital initiatives regarding parental presence and involvement. The second aspect focuses on the viewpoints and attitudes of both parents and healthcare professionals regarding physical closeness: what are their aspirations, and what constraints do they face?
Now, a new study published in Pediatric Investigation explores the current NICU scenarios to gain an overview into the practice of and hurdles to implementing zero-separation. "We wanted to draw up a comprehensive overview of current neonatal settings and explores the factors that enable and challenge parent-infant closeness during infant hospitalization in 19 countries," explains Ms. Nicole van Veenendaal of OLVG, Amsterdam, the first author of the study.
To maintain geographical and cultural diversity, at least two sample hospitals from each European country were included. Neonatologists experienced in caring for neonates less than 30 weeks of gestational age were selected from 11 countries. The participants from the selected 19 countries were interviewed using audio and video techniques, and their responses were analyzed to identify inter-related patterns in the data. These patterns or themes were then classified to reveal four distinct issues around parent-infant closeness: Culture, Collaboration, Capacities, and Coaching.
Culture, which encompasses the attitudes, behavior and values of the hospital staff, was found to be an overarching pattern that extended across the other three categories as well. The hospital culture was a major influencer of parental participation as it defined the levels of acceptance felt by the parents. The hospital staff at all hierarchical levels–from the top management to the unit staff including the nurses–displayed varying attitudes, which needed to be adjusted in order to create a uniform welcoming environment for the parents.
Collaboration refers to the cooperation between the medical staff from different units, as well as parent-staff collaboration. The cooperation between medical staff ensures smooth functioning of the NICU at all times, whereas the parent-staff teamwork was essential for issues like administering pain medication to the infants or for scheduling the daily rounds for parents.
Capacities such as availability of medical equipment and staff have a huge impact on parent-infant closeness. Simple logistical issues, like the distance of the NICU from the maternity ward, sometimes prevented mothers from spending more time with their infants. The presence of elaborate NICU equipment (leading to lack of space) and under-staffing issues were the other major hindrances in parent-infant closeness. Hospital policies like promotion of breastfeeding (including the use of breast pumps) and open access policies were also important factors in parent-infant closeness.
Coaching includes the training or skills needed to ensure parent-infant closeness. Coaching was done through well-defined training programs and covered the medical staff, NICU nurses and even midwives. A separate family coaching session was organized, to train the family members on the special care for their infant.
"Since this study includes the views of parents during the analysis phase, the results are relevant for all stakeholders," suggests Ms. van Veenendaal. While a lot still remains to be done in optimizing parent-infant closeness, the results of this study provides a promising pathway to the creation of a zero-separation model.
More information: Nicole R. van Veenendaal et al, An international study on implementation and facilitators and barriers for parent‐infant closeness in neonatal units, Pediatric Investigation (2022). DOI: 10.1002/ped4.12339