Tiny optical sensors could put an end to hospital bed sores
Tiny smart bed sensors embedded in hospital mattresses could put an end to painful and potentially life-threatening pressure sores, thanks to new technology developed by the University of South Australia.
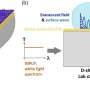
UniSA scientists have designed minute optical fiber sensors, which can be attached to the upper surface of a mattress to monitor movement and record heart and respiratory rates.
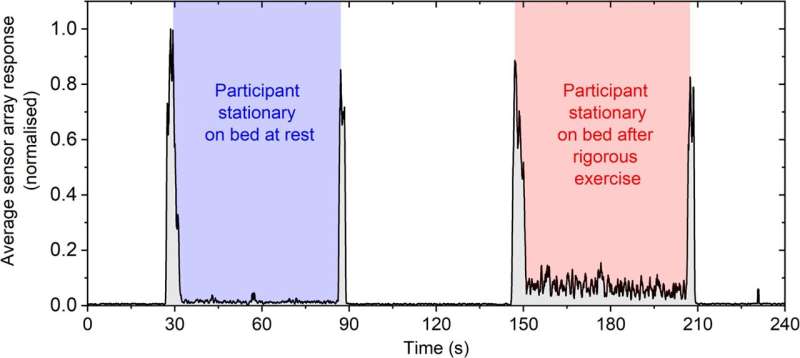
The unobtrusive sensors can detect when a hospital patient turns over, leaves a bed, or just remains motionless, picking up their breathing.
Nurses can therefore be remotely alerted if a patient has not moved within a couple of hours, prompting them to adjust the patient's position.
Lead researcher Dr. Stephen Warren-Smith says the technology could "significantly relieve" the burden on hospital staff having to constantly monitor patients for pressure sores.
"Each year, thousands of older Australians in hospitals and nursing homes experience pressure injuries, or ulcers, which take a long time to heal and can be fatal," Dr. Warren-Smith says.
"At the very least these injuries can cause severe pain, disrupt sleep, affect their mood as well as their rehabilitation, mobility and quality of life."
Unlike the sensors that many people wear on their wrists to monitor physical activity and physiological signs, the optical fiber sensors are embedded in the same space as a person, but not on them physically.
Hospitals currently use weight-based sensors or cameras installed in the room to monitor patients, but both have limitations, Dr. Warren-Smith says.
"Existing weight-based hospital sensors cannot predict when a patient leaves the bed until their feet touch the floor, leaving little time for nursing staff to respond in the event of a fall. Also, there are privacy issues with camera-based technology."
The optical fiber sensors are sensitive enough to record heart and respiration rates and can detect whether a person is in the bed, even if they remain stationary for long periods.
"Respiration rates are often the first sign that a patient is deteriorating. This normally requires devices to be attached to the patient, either on the chest, as a mask on the face, or ventilator. These can be restrictive and sometimes inappropriate in an aged care setting.
"Monitoring vital signs continuously, unobtrusively and cheaply via the mattress-embedded sensors is a far better solution for both patient and nurse," Dr. Warren-Smith says.
The technology is explained in a recent paper published in the Journal of Biomedical Optics.
More information: Stephen C. Warren-Smith et al, Multimode optical fiber specklegram smart bed sensor array, Journal of Biomedical Optics (2022). DOI: 10.1117/1.JBO.27.6.067002