Drug used for sleep disorders is linked to higher risk of overdose in teens, young adults
Teens and young adults who are treated for sleep disorders with benzodiazepines such as Xanax—a medication commonly prescribed to treat anxiety and insomnia—may be at a higher risk of overdose, according to Rutgers University researchers.
The study, published in JAMA Network Open, examined how often young people with sleep disorders had a drug overdose in the months after starting a prescription sleep medication.
According to the National Institute on Drug Abuse, benzodiazepines were involved in 12,290 overdose deaths in 2020, up from 6,872 in 2011 and 1,135 in 1999. However, Rutgers researchers said the risks of drug overdose in youth populations prescribed a benzodiazepine treatment for insomnia was unclear.
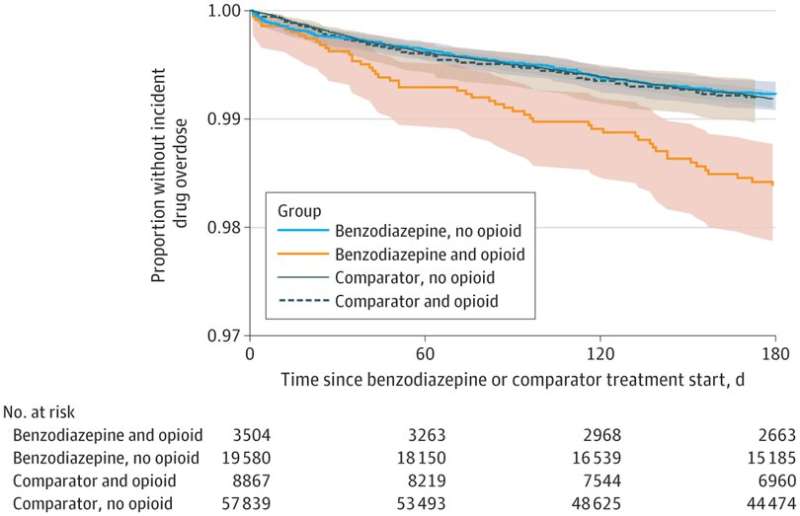
Researchers found young people using benzodiazepines for common sleep conditions had an increased risk of overdose during the six months after starting treatment compared with other prescription sleep medications, including trazodone, hydroxyzine and z-hypnotics.
"The risk of drug overdose with benzodiazepine treatment is an important safety consideration when treating adolescents and young adults," said Greta Bushnell, an author of the study and a faculty member at the Center for Pharmacoepidemiology and Treatment Sciences at the Rutgers Institute for Health, Health Care Policy and Aging Research (IFH). "We hope these results can inform prescribing decisions and encourage close monitoring in this young patient population."
Using a commercial claims database covering privately insured young people ages 10 to 29 years old, researchers identified nearly 90,000 people newly receiving benzodiazepine or an alternative prescription treatment for a sleep disorder. Researchers then examined drug overdoses in this group in the six months following the start of treatment.
Researchers also found the risk of overdose was highest among young people starting treatment with benzodiazepines who recently were prescribed an opioid.
"Given the frequent co-use of benzodiazepines with other substances, it is important to discuss with young people the potential associated harms," said Bushnell, who is an assistant professor at the Rutgers School of Public Health. "Because other substance use may be unknown to the prescriber, adolescents and young adults should be screened for substance use and a history of overdoses before treatment."
Bushnell said continued research is needed to determine how specific benzodiazepine treatment details, such as dosage, alter the risks of overdose.
Coauthors of the study include Tobias Gerhard of the Center for Pharmacoepidemiology and Treatment Sciences at IFH and the Ernest Mario School of Pharmacy at Rutgers and collaborating faculty at Columbia University Mailman School of Public Health, Columbia University Irving Medical Center and New York University School of Medicine.
More information: Greta A. Bushnell et al, Association of Benzodiazepine Treatment for Sleep Disorders With Drug Overdose Risk Among Young People, JAMA Network Open (2022). DOI: 10.1001/jamanetworkopen.2022.43215




















