Q&A: Cervical disk replacement
DEAR MAYO CLINIC: My husband has had terrible neck pain for a few years. It has gotten to the point where he cannot turn his head to either side enough to drive safely. We heard that replacing a disk in his neck might be the best option. Are there other things we should try first? And is this type of surgery safe?
ANSWER: Neck pain is a common problem, affecting many adults at some time in their lives. As in your husband's case, it can make simple activities, like driving a vehicle, painful or even impossible. The pain may involve just the neck and shoulders, or it may radiate down an arm. The pain can be dull or feel like an electric shock into your arm.
The Food and Drug Administration recently approved cervical disk replacement surgery as an alternative to spinal fusion. Like a knee replacement surgery, the artificial disk allows for full or nearly full range of motion after the surgery.
Our spines are a stacked column of two components: vertebrae and disks. Vertebrae are the bones in the spine, and disks are rubbery cushions that sit between the vertebrae.
The disks act as shock absorbers, allowing your spine and neck to bend, flex and rotate. The neck consists of seven vertebrae, called cervical vertebrae, and corresponding disks.
For some people, muscle strain causes neck pain. This could be a result of poor posture, carrying a heavy backpack or purse, cradling your phone between your shoulder and neck, or sleeping with too few or too many pillows.
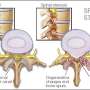
Neck pain also could be caused by structural changes to the cervical vertebrae or disks, like cervical spondylosis, spinal stenosis or a herniated disk. Often, neck pain responds to nonsurgical treatment, such as rest, steroid injection, stretching and massage. Surgery may be needed if pain continues, leads to neurological changes like weakness or numbness, or is accompanied by a structural issue.
In the past, the most common types of surgery on the cervical disks were spinal fusion and decompression surgery. During a spinal fusion, a spacer graft material is placed between two or more cervical vertebrae. Eventually, the vertebrae grow together, or fuse, over time.
Spinal fusion and decompression surgeries often are performed together. While these procedures are safe and relieve the pain, they permanently immobilize the spine and change the way the neck moves. Patients may no longer be able to turn their neck fully or look over their shoulders.
In addition, fusion can place additional stress and strain on the vertebrae above and below the fused portion. This could increase the rate of degeneration in those areas of your spine.
During a cervical disk replacement, the surgeon makes a small incision on the side or front of your neck. After other structures are moved to the side, your surgeon can access your spine. The worn-out disk is carefully removed and replaced with an artificial disk between two vertebrae. The artificial disk has two metal plates that are anchored to the roof and floor of the disk space to keep it in place.
Replacing a disk in the cervical spine may help relieve pain in the arms while maintaining motion and flexibility in the neck. It also decreases the stress on the remaining vertebrae. If your husband has facet joint disease or syndrome, he cannot have disk replacement surgery.
If your husband has a cervical disk replacement, you can expect that he will remain in the hospital one night and be encouraged to begin walking the day after surgery. Physical therapy will begin about six weeks after surgery. He also will have lifting and driving restrictions immediately after the procedure. It is important not to attempt to rush recovery, as the vertebrae and artificial disk need time to heal.—Dr. Navid Khezri , Neurologic Surgery, Mayo Clinic Health System, La Crosse, Wisconsin
©2022 Mayo Clinic News Network.
Distributed by Tribune Content Agency, LLC.