Tailored online personal health record cancer tool increases survivor adherence to national guidelines
Use of the Personal Health Record for Colorectal Cancer Survivors, a new online tool specifically tailored to meet the needs of and make support available for the more than 1.5 million individuals in the U.S. with a history of colorectal cancer, produced a significant increase in adherence by survivors to national guidelines recommending critical follow-up, especially colonoscopy surveillance and blood work.
A feasibility study from Regenstrief Institute, the VA, and Indiana University's schools of medicine and nursing research scientists validates functionality of the patient-centered tool they developed, opening the door for their larger study of the tool's use by those navigating the path forward following colorectal cancer surgery.
Unlike electronic health records, which are managed by clinicians and healthcare systems, the Personal Health Record for Colorectal Cancer Survivors is controlled by the survivors themselves. The online tool is securely available when and where the survivor wishes to access it to view contents or add information.
This personalized focus enables colorectal cancer survivors to track, help manage and mitigate the impact of their disease—given its specific location and stage as well as other medical conditions and current treatment.
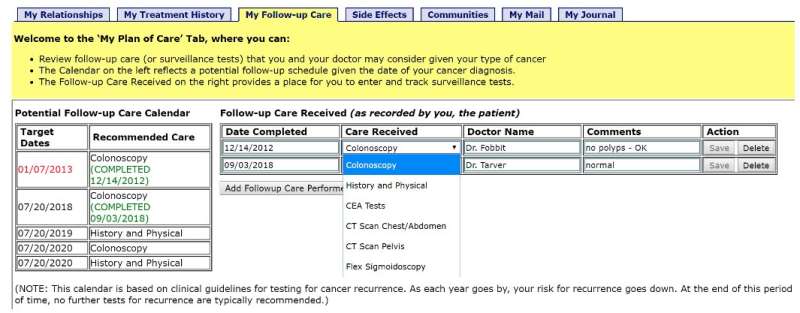
Features of the tool include an updateable summary of cancer treatment history, a follow-up care and surveillance schedule, reminder functions, identification of role-based individuals (primary care physician, oncologist, social worker, caregiver) with whom they may wish to share all or portions of their personal health record, specifics on side effects of prescribed medications, community resources and other useful, personalized functions—such as a secure message capability—which enables patients to send and receive messages from individuals with whom they have created a relationship. This might include clinicians, family members, friends or other colorectal cancer survivors.
The Personal Health Record for Colorectal Cancer Survivors also provides survivors with the opportunity to enter information about symptoms they may be experiencing—for example, pain, anxiety, depression, sleep problems, fatigue—and generates a timeline tracking the intensity of the symptoms over the short and long term.
Based on this information, the tool provides them with tips or self-management approaches to address those symptoms at home, or, if the symptoms reach a high-level of severity, the tool guides them to connect with their providers.
"This is a system that we built leveraging OpenMRS, an open source electronic medical record system platform developed at the Regenstrief Institute, and tailored it to respond to and meet the specific needs of colorectal patients and survivors. It's really a shift in who has access, even ownership of the survivor's health record," said Regenstrief Institute Center for Health Services Research Director David Haggstrom, M.D., MAS, senior author of the new study and co-designer of the online tool.
"Combining patient-centered design with our extensive experience with doctor-patient communication and electronic medical records we saw an increase in adherence to national guidelines recommending critical follow-up by colorectal cancer survivors using the tool."
According to the American Cancer Society, approximately one in 23 men and one in 25 women in the U.S. will be diagnosed with colorectal cancer in their lifetime. For many, their cancer will reoccur after surgery underscoring the critical need for post-procedure follow-up. The World Health Organization lists colorectal cancer as the second most common cause of cancer death in the world in 2020 with 916,000 fatalities.
The tool is focused on activating survivors, giving them the ability and confidence to play a role in managing their own care when faced with a potentially life-threatening disease. Going forward, the researchers will explore ways for users to integrate the tool into their stressful lives and plan to work with clinicians and administrators on how this patient-centered technology can potentially be paired with the patient's electronic health record.
"The general framework that we've taken with colorectal cancer survivors is one that can serve as a guide for designing technologies for other cancer populations or types of cancer. But, in my experience, the clinical details and unique needs of different types of cancer require different approaches," said Regenstrief Institute Research Scientist Eric Vachon.
"I think that there is a huge opportunity to implement personal health records among all types of cancer more widely and to design and test them for the many types of cancer there are. When people think about cancer, they often think of a large monolithic disease, and along with heart disease, cancer is indeed one of the two most prevalent diseases among the U.S. population. But cancer is many diseases and they all require their own unique approaches, so there is much work ahead of us all—clinicians, research teams, patients and caregivers."
According to the Centers for Disease Control and Prevention (CDC) one in three people living in the U.S. will have some type of cancer during their lifetime. Approximately 600,000 people in the U.S. die of cancer annually.
The research is published in JMIR Cancer.
More information: Eric Vachon et al, Impact of a Personal Health Record Intervention Upon Surveillance Among Colorectal Cancer Survivors: Feasibility Study, JMIR Cancer (2022). DOI: 10.2196/34851