This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
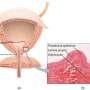
Dangers of late cervical cancer diagnosis in women of color

In the past decade, nearly one-third of cervical cancer cases in the U.S. resulted in death according to the Centers for Disease Control and Prevention. Women of color, particularly Hispanic and non-Hispanic Black women, are more likely to be diagnosed and die of cervical cancer compared to white women in the U.S.—not because of genetics, but inequalities in health care access.
Access to health care and establishing trust is essential to help reduce cervical cancer mortality.
Dr. Olivia Cardenas-Trowers, a Mayo Clinic urogynecologist, says limited access to transportation, education and other factors have created barriers to health care, particularly in communities of color.
"Removing barriers so that these women can have access is critical," says Dr. Cardenas-Trowers. "Then, when they are in the system being with providers they can trust, they can communicate if they have problems or need access to things like pap smears or other screening measures."
There is a greater chance at a cure when cervical cancer is detected early, when there may not be any noticeable symptoms—making regular screenings that much more important.
"It's really in later-stage cervical cancer where you can see things like abnormal vaginal bleeding, pain—in general or with intercourse," says Dr. Cardenas-Trowers.
The biggest risk factor for developing cervical cancer—HPV infection—can be prevented with a vaccine.
"Establish care with a primary care provider, undergo the recommended screening. Get the HPV vaccine for yourself if you're eligible and also for your children," says Dr. Cardenas-Trowers.