This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
AI provides personalized guidance based on inherited risk of heart disease
Researchers demonstrated that a causal artificial intelligence (AI) system can accurately quantify how much a person must reduce their blood pressure or low-density lipoprotein (LDL) cholesterol to overcome their inherited risk of coronary artery disease (CAD), according to research presented at the American College of Cardiology's Annual Scientific Session Together With the World Congress of Cardiology.
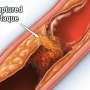
CAD is a form of heart disease caused by the buildup of plaque from LDL, or "bad" cholesterol, in the arteries, limiting blood flow to the heart. Causal AI is designed to help explain cause and effect of why a person is at risk, how to reduce that risk and how much they will benefit from specific actions to reduce risk. The study is the first to combine causal AI with a polygenic risk score for CAD to quantify how two key modifiable heart disease risk factors—blood pressure and LDL cholesterol levels—can be used to help guide people on how to overcome their inherited risk of CAD.
According to the findings, polygenic risk (a metric capturing a person's risk of heart disease based on their genes) is a relatively weak risk factor for most people that can be easily overcome with relatively modest reductions in blood pressure and LDL cholesterol. However, since the impacts of high blood pressure and LDL cholesterol accumulate over time, the amount of reduction needed to overcome polygenic risk is higher the later this reduction is achieved. Researchers said the AI system can be used to provide clear goals for each person along with guidance on steps needed to achieve them at all ages across their lifespan.
"The breakthrough of causal AI is that it quantifies all of these recommendations and personalizes them so each person can know exactly how much they need to lower their LDL, their blood pressure or both to overcome their inherited risk," said Brian A. Ference, MD, MPhil, MSc, professor and director of translational therapeutics at the University of Cambridge in the United Kingdom and the study's lead author. "It's much more motivating and powerful to persuade people to invest in their health if you can explain to them how they can reduce their risk and how much they'll benefit from the recommended actions, rather than simply telling them what their risk is."
Polygenic risk scores capture a person's genetic risk for heart disease by combining the risk conferred by millions of genes into a single number. To test whether this metric can be useful for informing patient care at the individual level, the researchers first used randomized data from clinical trials and genetic studies involving 1.8 million participants to train a causal AI system to estimate the effect of blood pressure and LDL on the risk of major coronary events. They then calculated polygenic risk scores for over 445,000 participants in the UK Biobank dataset and used the AI model to estimate how much each participant with higher-than-average polygenic risk must lower their blood pressure, LDL cholesterol or both to reduce their risk of major coronary events to the same level as people with average polygenic risk, blood pressure and LDL cholesterol.
The researchers then validated the system's accuracy by comparing its estimates to the observed risk of major coronary events in people with different levels of polygenic risk who by Mendelian randomization (an analysis method that uses genetic variation to investigate causal relations between modifiable risk factors and health outcomes in observational data) had higher or lower LDL, blood pressure or both. The results showed that the system performed well, and the findings suggest that even people with a very high genetic predisposition to heart disease can overcome that genetic predisposition by keeping their blood pressure and LDL cholesterol in check.
"This approach transforms AI into something we can think about using in clinical medicine because it is explainable and can be tested using randomized evidence," Ference said. "It empowers people with specific, actionable information and goals. This can not only help guide physicians and patients, it can even help governments and health care systems set more rational policy about how to incorporate polygenic risk into clinical medicine and public health policies."
The researchers also found that family history of heart disease is independent from polygenic risk and a much stronger predictor of major coronary events than polygenic risk for most people. Therefore, combining polygenic risk with family history can provide a better picture of a person's inherited risk than polygenic score alone.
The causal AI system is being made available in a free app (www.deepcausalai.org), which the public or clinicians can use to calculate a person's inherited risk of heart disease and get customized blood pressure and LDL cholesterol targets. A real-world, adaptive, cluster-randomized trial to assess whether the tool can help reduce the risk of heart disease will begin later this year.
The study was based on participants who self-identified as being of European ancestry. However, because AI encodes biological cause and effect, the researchers believe it can help guide clinical care using polygenic scores from any ethnic group. The investigators hope that this will motivate the development of more robust polygenic scores to help personalize the prevention of CAD in other ethnic groups.