This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Stigma-coping intervention empowers people with HIV and drug use to engage in health, substance use care
Stigma negatively impacts the health of people with human immunodeficiency virus (HIV) and those with HIV who inject drugs experience stigma on multiple levels. Stigma leads to impaired utilization and retention in addiction treatment, less access to harm reduction services and reduces HIV care success. Unfortunately, there is a lack of interventions specifically targeting stigma related to HIV and substance use among people with HIV who inject drugs.
Now a new study from Boston University Chobanian & Avedisian School of Medicine has found that a brief stigma intervention that specifically targets people with HIV who inject drugs was effective in increasing engagement in substance use care as well as improving their ART adherence. The project was a US/Russia/Ukraine collaboration preceding the escalation of the war last year.
"Our findings reinforce that in settings where stigmatizing attitudes remain pervasive, stigma-coping interventions empowering affected people can attenuate stigma's impact on substance use and HIV care," explains corresponding author Karsten Lunze, MD, MPH, DrPH, associate professor of medicine.
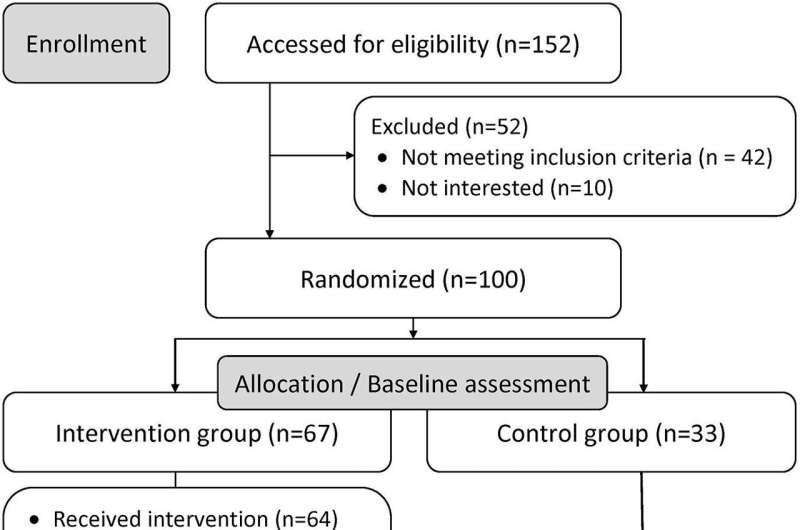
The researchers engaged leading stigma intervention experts and community organizations in Russia and Ukraine and together developed anti-stigma group sessions. The group then recruited 100 participants with HIV and past-30-day injection drug use at community outreach buses run by a non-governmental harm reduction organization in St. Petersburg, Russia. The study participants were randomized to receive either usual services only or an additional intervention of three weekly two-hour group sessions.
The researchers found that the intervention group participants had higher chances to start ART (20% vs 3% compared to the non-intervention) and engage with substance use treatment (23% compared to 7%).
According to the researchers, the increase in engagement might be due to the acceptance-based nature of the intervention, i.e., the reduction in avoidance of health care settings. "The intervention was not intended to directly reduce shame and fears related to internalized societal stigma, but was rather focused on improving stigma coping and thereby increasing healthy behavior and care seeking," said lead author Jason Luoma, Ph.D., from the Portland Psychotherapy Clinic, Research, and Training Center.
These findings appear online in The Lancet Regional Health—Europe.
More information: Jason B. Luoma et al, An acceptance-based, intersectional stigma coping intervention for people with HIV who inject drugs—a randomized clinical trial, The Lancet Regional Health—Europe (2023). DOI: 10.1016/j.lanepe.2023.100611