This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Study finds Medicaid telemedicine coverage boosted use, healthcare access
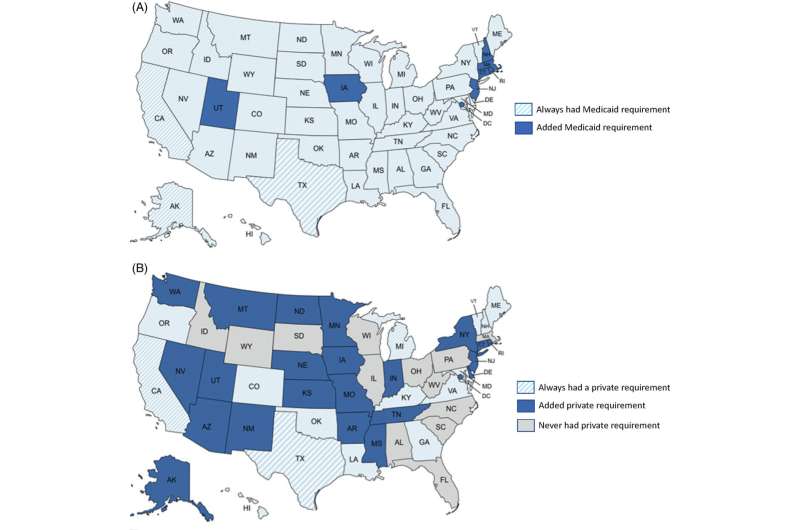
Medicaid telemedicine coverage between 2013 and 2019 was associated with significant growth in telemedicine use and improved healthcare access, while private policies did not have such an association, according to a study led by the University of California, Irvine.
An analysis of 20,000 records of U.S. adults under 65 with either state-level Medicaid or private policies showed that live video chats increased by 6 percentage points and that the ability to consistently access necessary care increased by 11 percentage points for Medicaid patients.
Recently published online in the journal Health Services Research, the findings were based on nationally representative data from the Association of American Medical Colleges' Consumer Survey of Health Care Access.
"The results highlight the positive impact of Medicaid telemedicine coverage during the study period and have important implications for policymakers as they navigate decisions now that the COVID-19 public health emergency has ended," said corresponding author Brandy Lipton, Ph.D., associate professor of health, society & behavior in UCI's Program in Public Health.
"With many states having implemented or expanded telemedicine protection during the pandemic, our study provides valuable insights that can inform policymakers' decision-making efforts moving forward."
Telemedicine requirements for Medicaid and private insurers are determined at the state level, leading to a diverse landscape of policies across the country, with reimbursement rates and cost-sharing arrangements for virtual and in-person services that vary across insurers. Researchers found that Medicaid enrollees reported greater unmet health needs and lower utilization, on average, than the privately insured, despite lower levels of cost sharing for most services.
This disparity may be due to higher barriers to access for this population, including transportation limitations, less English proficiency, advanced age and functional limitations.
"Our investigation into the relationship between state policies and healthcare usage and access underscores the tremendous potential telemedicine has to help overcome barriers and improve health outcomes for all individuals, regardless of their social or demographic circumstances," Lipton said. "Understanding the role of state policies in telemedicine use and access will prove instrumental in shaping future policymaking efforts as the healthcare landscape continues to evolve beyond the pandemic."
More information: Brandy J. Lipton et al, State Medicaid and private telemedicine coverage requirements and telemedicine use, 2013–2019, Health Services Research (2023). DOI: 10.1111/1475-6773.14173