This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
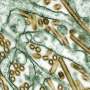
Could bird flu spark the next pandemic, and are we prepared if it does?

Scientists always knew a deadly virus was going to jump from animals to humans: COVID was not the first time it has happened, and it won't be the last. Should we be worried about frequent news reports of flu being detected in birds and other animals?
In Hong Kong in 1997, eighteen people were infected with bird flu. Six of them died. This was the first time the highly infectious disease H5N1 had ever been seen in humans—and it raised the alarm.
"From that moment, influenza researchers studying animal to human transmission suddenly became much better funded," says Professor Derek Smith, Director of the Center for Pathogen Evolution at the University of Cambridge. "The strain of bird flu in Hong Kong was killing a third of the people it infected. If that could start transmitting directly between humans, it would be a disaster."
Bird flu is considered by the World Health Organization to be a major pandemic threat. And the world is currently experiencing the worst bird flu epidemic ever seen.
Over the last year there have been more outbreaks of bird flu on farms—killing chickens, ducks and turkeys—than ever before. Over 140 million poultry have died worldwide from the disease or related culling since October 2021, according to the World Organization for Animal Health.
"We used to think that five outbreaks in a season was bad, but hundreds of UK farms have gone down with bird flu in the last twelve months," says Professor James Wood, Head of the Department of Veterinary Medicine at the University of Cambridge.
"It kills farmed birds really fast—they're usually dead within 24 hours of showing signs of infection, and we're seeing mass mortality events," he adds.
Like COVID, there isn't just one strain of bird flu. This latest strain is unusually fatal in a wide range of bird species and unusually transmissible between bird species.
It isn't clear where the virus came from, but it's clear that a recent huge epidemic in wild birds has been causing the infections on farms, putting pressure on farmers and threatening our food supply.
"Disease on this scale in wild birds in Europe has never been seen before," says Wood.
"It's been absolutely devastating," he adds, "pushing some species to the brink of extinction. Gannets, terns, and cranes have all died in huge numbers. Lindisfarne, for example, was recently closed to the public because of the amount of wild bird disease on the island."
Wood leads the University's involvement in a new national consortium called FluMap, which brings together eight of the UK's top scientific organizations. The group aims to better understand the strain of H5N1 causing this unprecedented bird flu outbreak—and find ways to tackle it. Their results will feed into government decision-making, and new strategies to protect the poultry industry and reduce the risk of future transmission to humans.
Wild birds typically spread bird flu to farmed birds by direct contact, or through feces in farmyards or feed stores.
Cambridge's role in FluMap is to survey biosecurity on UK poultry farms aimed at preventing infections in farmed birds. "We're trying to understand what people really do, and why," says Wood.
"Poultry farmers need to make sure their birds don't come into contact with wild birds, by using netting or keeping them indoors. They can try and keep wild birds away with bird scarers, and not having ponds to attract them," he says. "They also need to stop wild bird feces being transferred in—by cleaning boots, or putting on new ones every time they go into a poultry shed."
"It's not high-tech, it just takes a lot of effort all day long. Often where there have been bird flu outbreaks on farms it's an issue with biosecurity—so in part it's a human failure."
Outbreaks on farms seem to have seasonality, linked with the migration patterns of wild birds. And because birds can fly, the outbreak has now gone global. Scientists don't currently understand the infection dynamics in wild bird populations, which makes ongoing surveillance vital.
The UK government's asymptomatic testing program has so far detected very few cases of the current bird flu in humans.
In most cases, the person first infected by an animal virus was in very close contact with the animal. This usually happens most in less developed parts of the world.
"When you look at the scale of the latest bird flu epidemic on European farms, I think it's remarkable how few human cases there have been," says Wood. "I'd argue that this strain is not well adapted for transmitting into humans, because people working on poultry farms are exposed to bird flu all the time."
But a variant of bird flu more closely related to the one that killed humans in Hong Kong is still circulating in Cambodia and the Far East. There's also concern about the variant transmitting in Europe and the Americas because it has jumped, or "spilled over," into various other animal species. Several cases have been seen in foxes—which eat dead birds, and there have been outbreaks in seals and sealions in Peru and on mink farms in Spain.
Mammals are more closely related to humans than birds, so are more likely to transmit the virus to us. Bats, rats, civet cats, widgeons, and even camels are known to carry pathogens that can jump to humans.
"The worry is that some of the mutations associated with better transmission in humans have been picked up in some of these mammalian species," says Wood.
The deadly Spanish flu pandemic of 1918 infected a third of the world's population, killing an estimated 50 million. It is believed to have been caused by a bird flu that jumped to humans.
Since the Hong Kong outbreak, H5 and related H7 bird flu viruses have been spreading globally. Several hundred cases have been detected in humans: 50% of those infected have died.
It's much harder for one person to catch the virus from another, because they would inhale a much lower dose than the original person who was infected.
"But given how deadly bird flu is, there's huge concern about it transmitting between humans," says Smith.
Once a person is infected, the virus must evolve to replicate in humans and escape our immune system. This allows it to start spreading between people, causing the chain reaction that leads to a pandemic.
Smith has developed a technique called "antigenic cartography," which uses data from virus samples collected by labs around the world to study how bird flu and other viruses are evolving. This includes viruses that are continually getting into humans, but haven't yet managed to spread from one person to another.
"We look at how well human antibodies, formed in response to infection with one virus, respond to infection with a variant of that virus," says Smith. "This tells us whether a virus has changed enough to escape the human immune response and cause disease, potentially sparking a pandemic."
For Smith, being prepared for the next pandemic is all about vaccines.
Many developed countries already have H5 vaccine stockpiles ready. His world-leading work helps determine—on an ongoing basis—whether these vaccines are likely to be protective, or whether they need to be updated. As we know from COVID, variants continue to emerge just as we develop vaccines to try and stop the spread.
"We want to know the key virus variants to make vaccines against, to be better prepared for future pandemics. Some are quite closely related, so the aim is to make vaccines that give broad immunity against many variants," says Smith.
Smith has studied human influenza for 30 years to understand its evolution and how it escapes immunity, and whether this can be predicted. His technique is now used in the World Health Organization's process of choosing which variants go into the annual flu vaccine.
He also uses flu as a model for other pathogens that are harder to study in the lab. This was part of the huge amount of preparatory research, across many institutions, that enabled such a rapid response when COVID emerged in humans in 2019.
"The response to COVID-19 looked like chaos, but the truth is the world did well in the pandemic—and it will do even better next time," says Smith.
"The speed at which tests were developed, and vaccines were produced, and clinicians figured out the best way to treat COVID was thanks to all the work done below the radar for the past twenty years—much of which was in preparation for a severe flu pandemic."
By using antigenic cartography to compare the similarity of virus variants as they emerge, Smith is confident that current vaccines can be updated to work against future variants.
"Vaccines are our best protection—they saved the most lives in the COVID pandemic," he says. "There's no reason why they can't be made at least that quickly for future pandemics—and there will be another flu pandemic for sure."