This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Immunotherapy for brain cancer metastases shows clinical benefit
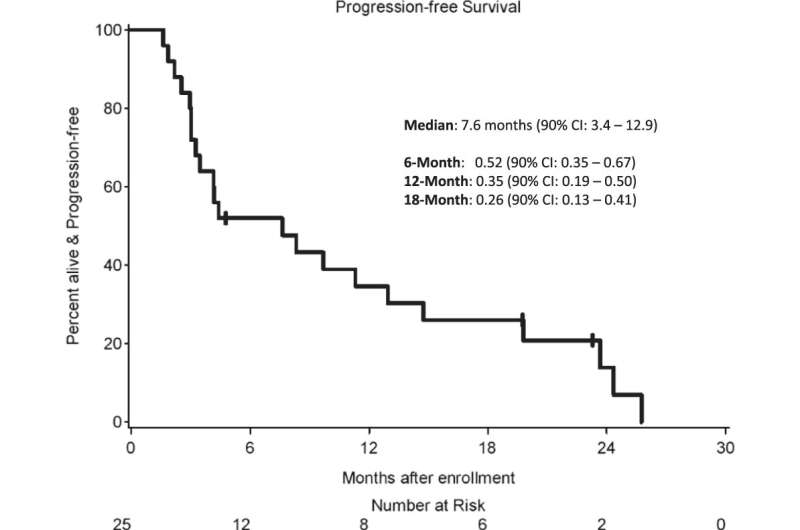
In a phase 2 clinical trial of the immune checkpoint inhibitor pembrolizumab, investigators found that 42 percent of patients with metastatic brain cancer benefited from the therapy, with seven patients in the trial surviving longer than two years.
The authors caution that these benefits must be weighed against risk of toxicity, but, overall, the study shows promising results that warrant larger studies and efforts to identify patients most likely to benefit from this treatment. Their findings are published in Nature Medicine and presented simultaneously at the 2023 ASCO Annual Meeting on June 2.
"There are very few effective treatments for patients with brain metastases. Our overarching objective is to find improved therapies for this patient population," said corresponding author Priscilla K. Brastianos, MD, of the Mass General Cancer Center. "With this trial, we investigated pembrolizumab, which is an immunotherapy for patients with brain metastases. We showed that pembrolizumab was tolerated and showed clinical benefit in the brain in 42 percent of patients, which is promising for this patient population."
The single-arm, open-label, phase 2 trial included nine patients with previously untreated, asymptomatic brain metastases (cohort A) and 48 patients with recurrent and progressive disease after prior therapy (cohort B). Participants were enrolled in the trial between Oct. 6, 2016 and Oct. 16, 2018.
The primary endpoint of the study was response rate, including complete response, partial response, or stable disease. Patients in the trial had primary tumor diagnoses that included breast, melanoma, non-small cell lung, small-cell lung, pituitary, and other cancers.
The research team found that 24 of the 57 patients had an intracranial benefit, with five patients experiencing a complete or partial response to treatment. This included three patients in cohort A and 21 in cohort B, meaning the study achieved its primary endpoint.
The team also reported that median overall survival for participants was 8 months. While the study did not have a control arm, previous studies have estimated overall survival for patients with brain metastases to be 4-6 months. Seven patients in the study experienced prolonged overall survival of two or more years, including five patients with primary breast cancer, one patient with primary melanoma and one patient with primary sarcoma.
The team also examined safety and tolerability. Five patients discontinued treatment due to toxicity, and 50 of the 57 patients had one more adverse event. The most frequent adverse events were fatigue, nausea, headache, vomiting and transaminitis (elevated levels of liver enzymes in the blood).
As next steps, the research team recommends investigating biomarkers of response, especially among the study's "exceptional responders," that may help to predict which patients are most likely to respond to therapy. The authors note that additional studies will be needed to identify specific facets to those patients' tumors or tumor microenvironments that led to such a favorable response.
"Our study illustrates the promise of checkpoint inhibitors for future therapeutic strategies for brain metastases," said Brastianos. "And our work suggests that the decision to give a checkpoint inhibitor should not be based solely on the primary tumor's origin—it is likely that there are yet-to-be determined factors that may predict response. Future studies to identify these factors may help guide, inform, and personalize treatment for patients with brain metastases."
More information: Brastianos, P.K. et al, Pembrolizumab in brain metastases of diverse histologies: phase 2 trial results, Nature Medicine (2023). DOI: 10.1038/s41591-023-02392-7. www.nature.com/articles/s41591-023-02392-7