This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Kenyan hospital visits linked to increased exposure to antibiotic-resistant bacteria
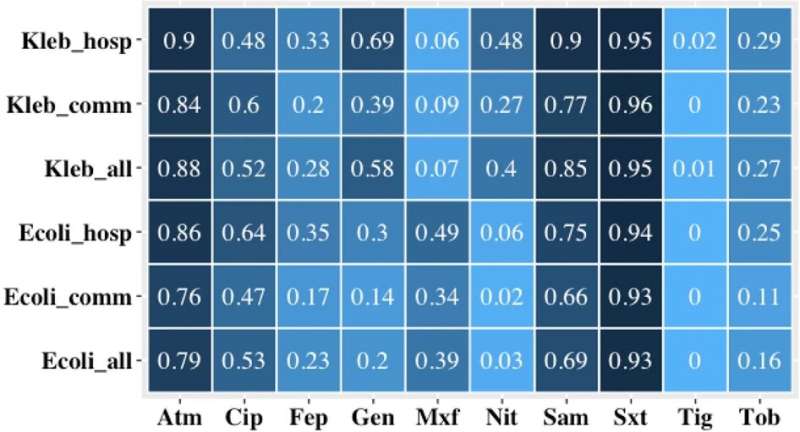
Kenyan patients who spend more than three days in the nation's hospitals are more likely to harbor a form of bacteria resistant to one of the most widely used antibiotic classes, according to a recent study led by Washington State University.
The research team found that 66% of hospitalized patients were colonized with bacteria resistant to third-generation cephalosporins, compared to 49% among community residents. Third-generation cephalosporins are typically used for serious infections, and resistance to these antibiotics leaves limited options for treating patients with some bacterial infections.
The study, published in the Clinical Infectious Diseases journal, was part of a pair of projects in Kenya and a third in Guatemala to determine the prevalence of antibiotic-resistant bacteria. The research also aimed to identify risk factors for colonization with bacteria resistant to important and frequently used classes of antibiotics, including third-generation cephalosporins.
"These bacteria can cause untreatable infections," said Sylvia Omulo, an assistant professor at WSU's Paul G. Allen School for Global Health who led the studies in Kenya. "We have to use surveillance to make sure we understand what causes these bacteria to colonize and, later, resist certain antibiotics."
By examining health records of Kenyan hospital patients who were colonized with cephalosporin-resistant bacteria, researchers identified three risk factors associated with colonization. Those risk factors included hospitalization for more than three days at 132% increased risk, intubation at 73% and a positive HIV status at 70%.
A person colonized with the bacteria may show no symptoms of an infection; however, the germs are present and growing in their body, and the individual may be at increased risk of a more dangerous infection from something as simple as a minor medical procedure or sickness from common bacteria like E. coli and Klebsiella. The germs can unknowingly be spread through person-to-person contact or contaminated surfaces.
While resistance is often associated with improper antibiotic use, that does not appear to be a primary contributing factor for cephalosporin-resistant bacteria in either Kenya or Guatemala.
The Guatemala study, led by WSU Allen School assistant professor Brooke Ramay, was interrupted by the COVID-19 pandemic and resulted in data being collected during two time periods. Reported antibiotic use in the community declined three-fold between the pre- and post-periods, but the prevalence of cephalosporin-resistant bacteria remained steady, with colonization found in 67% of hospital patients and 46% of community subjects.
"If antibiotic use locally in the community was a major risk factor, we'd expect some change over the course of the year," said WSU Regents Professor Douglas Call, corresponding author for the three publications.
In a Kenyan study of communities, the likelihood of colonization with cephalosporin-resistant bacteria rose by 12% with increasing visits to hospitals and clinics, and individuals who kept poultry were 57% more likely to have the resistant bacteria. Previous and ongoing work in both countries also highlights the role of bacterial transmission due to poor sanitation and hygiene.
What is not clear is if contact with the health care system is a source of transmission or if people seeking care are more likely to harbor these bacteria.
"We know if you're interacting with the health care system, you're more likely to carry these bugs, but we don't know why yet," Call said. "To sort out the cause from the effect, we need to track the same people over time and record how their colonization status changes with different behaviors. Studies to do this are being set up for the coming year."
More information: Sylvia Omulo et al, Risk factors for colonization with extended-spectrum cephalosporin-resistant and carbapenem-resistant Enterobacterales among hospitalized patients in Kenya: An Antibiotic Resistance in Communities and Hospitals (ARCH) study, Clinical Infectious Diseases (2023). DOI: 10.1093/cid/ciad258