This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Big blood savings: Large trial shows taking less blood for lab testing reduces transfusions in intensive care
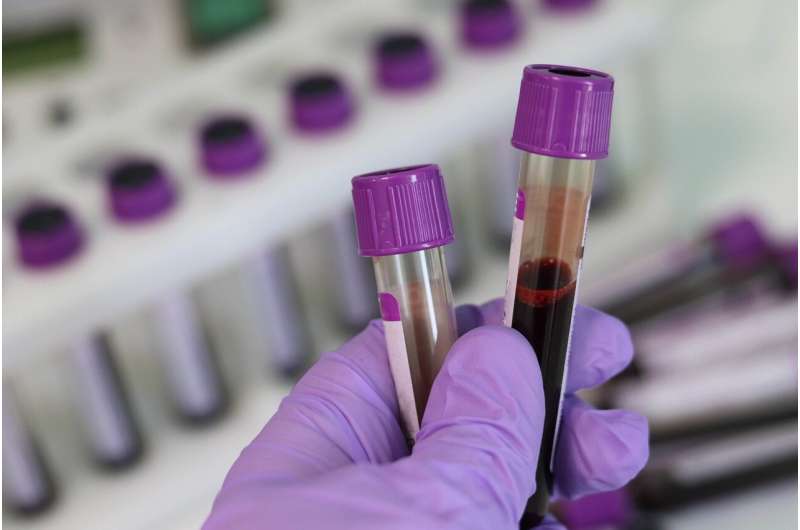
A world-first clinical trial published in JAMA could provide an easy way to save tens of thousands of units of blood every year in Canada and much more worldwide.
The trial, which involved more than 27,000 patients in 25 adult intensive care units (ICUs) across Canada, showed that taking less blood for lab tests using "small-volume" tubes reduced the need for almost one blood transfusion for every 10 patients.
Most hospitals use standard tubes that automatically draw four to six milliliters (ml) of blood, but a typical laboratory test requires less than 0.5 ml of blood, meaning the rest (more than 90%) is wasted. Commercially available small-volume tubes have a weaker vacuum inside that automatically draws up to half as much blood.
"While the amount of blood drawn per tube is relatively small, ICU patients typically require multiple blood samples taken multiple times every day. This can add up to significant blood loss that contributes to anemia, or low red blood cells. ICU patients are unable to produce more red blood cells to correct for this blood loss and often require treatment with a blood transfusion," said senior author Dr. Deborah Siegal, a scientist and hematologist at The Ottawa Hospital who led the trial, which was coordinated by the Population Health Research Institute (PHRI) in Hamilton, a joint institute of McMaster University and Hamilton Health Sciences.
"This trial showed that we can save one blood transfusion for every 10 ICU patients by simply switching to small-volume tubes for blood collection," said Dr. Siegal, who maintains appointments with McMaster University and PHRI, in addition to the University of Ottawa.
"At a time when everyone is trying to find ways to make health care more sustainable, and preserve our supply of blood products, this study provides a simple solution that can be implemented without additional cost or negative effects. The patients in our study received over 36,000 blood transfusions. With small-volume tubes we may have saved about 1,500 units of blood."
In Canada, the costs associated with blood transfusions ($450 per unit of blood, with additional costs to hospitals for testing, preparation, storage, etc.) are covered by the public health system. Blood donors are not paid, and blood conservation is a priority as shortages are common.
The study also has important implications for patients, as low red blood cells (anemia) can leave patients feeling tired and weak and is associated with can lead to other complications and longer hospital stays. While blood transfusions can usually correct anemia, there can be rare side effects, such as difficulty breathing, allergic reactions and infections.
The trial employed an innovative design that involved randomizing different ICUs to use either small-volume blood collection tubes or regular tubes for different periods of time, before switching to the other tubes. The researchers used electronic medical records to track how many blood transfusions were given to each patient, excluding patients who stayed for less than 48 hours in the ICU.
While previous observational studies have supported the use of small-volume tubes, this is the first clinical trial to rigorously test them in the hospital setting. In addition to finding that the small-volume tubes reduced anemia and the need for blood transfusions, the trial also confirmed that the smaller volume of blood did not compromise laboratory testing. When the researchers excluded results from the height of the pandemic (five months of data), the trends were the same, but did not reach statistical significance.
By the numbers
- 97: Percentage of patients who develop anemia after eight days in the ICU
- 50: Percentage of transfusions given in the ICU in the absence of active bleeding
- 41: Amount of blood (in ml) taken per ICU patient per day for routine blood tests (equivalent of one full blood donation every eight days)
- 75: Percentage of patients who receive at least one blood transfusion within seven days of ICU admission (40% of all ICU patients)
- $450: Cost per unit of blood in Canada (not including indirect costs associated with testing, preparation, storage, administration, reactions)
- 90: Percentage of blood that is wasted in routine lab tests
- 10: Units of blood that could be saved per 100 patients with ICU stays of more than 48 hours if the results of this study were implemented
More information: Small-Volume Blood Collection Tubes to Reduce Transfusions in Intensive Care, JAMA (2023). DOI: 10.1001/jama.2023.20820. jamanetwork.com/journals/jama/ … 1001/jama.2023.20820