October 19, 2023 feature
This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Solving a malaria mystery: Vessel congestion may drive brain swelling in children with cerebral malaria
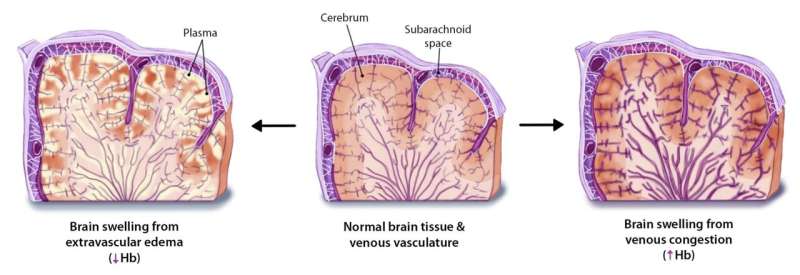
Unusually high levels of blood congestion in vessels feeding the brain may lead to severe swelling, scientists have found in a discovery that solves a longstanding malaria mystery: how the infection deleteriously impacts the brain of children.
Malaria is a staggeringly relentless and insidious infection, a mosquito-borne disease that infects an estimated 219 million people annually and claims 400,000 lives, mostly children under the age of five, according to the World Health Organization.
One of the most difficult-to-treat complications in pediatric malaria is swelling of the brain, which is marked by fluid accumulation and vascular congestion of red blood cells. The problematic swelling can lead to coma, and in many cases, death.
The disease itself occurs with the bite of a blood-sucking female Anopheline mosquito when its proboscis—a veritable hypodermic needle—pierces a blood vessel and transmits protozoan parasites. Four species of Plasmodium protozoa exclusively infect humans who serve as intermediate hosts in the parasites' development. The four protozoan species are: Plasmodium falciparum; P. vivax; P. ovale and P. malariae. Of the four, P. falciparum causes the most devastating manifestations of the disease.
Scientists in the Laboratory of Malaria and Vector Research at the National Institute of Allergy and Infectious Diseases in Bethesda, Maryland, have been conducting research to determine the cause of pediatric brain swelling triggered by malarial infection. All of the children in the study were from Malawi and infected by P. falciparum, which dominates on the African continent.
Currently, there are two dueling hypotheses that hold sway over the cause of brain swelling in cerebral malaria. The first contends the swelling arises from cerebral edema, excess fluid that dangerously collects in the brain. The second implicates "sticky" red blood cells that obstruct blood flow in brain vessels. Regardless of which is correct—and the new investigation was designed to find the answer—the hope was to better understand this life-threatening manifestation of malaria.
Reporting in Science Translational Medicine, Dr. Rachel L. Smith in the physiology unit of the Laboratory of Malaria and Vector Research at NIAID, knew it would require sophisticated imaging technology to help uncloak the cause of this potentially lethal complication. Working with colleagues at Queen Elizabeth Central Hospital and Blantyre Malaria Project of Kamuzu University in Malawi, researchers emphasized that their investigation would open a new window of understanding into malaria's impact on the brain.
"Brain swelling is associated with death from cerebral malaria, but it is unclear whether brain swelling is caused by cerebral edema or vascular congestion—two pathological conditions with distinct effects on tissue hemoglobin concentrations," Smith wrote in Science Translational Medicine.
"Cerebral edema is associated with increased brain tissue water content and intracranial pressure as well as compression of small blood vessels, which lowers cerebral hemoglobin concentrations. In contrast, in venous obstruction, blood vessels become engorged with blood, resulting in an increase in cerebral hemoglobin concentrations," Smith asserted. "We used near-infrared spectroscopy to noninvasively study cerebral microvascular hemoglobin concentrations in 46 Malawian children with cerebral malaria."
All together, 108 children were involved in the research project, which included healthy children who took part in the study as controls. As a result of their research, Smith and colleagues were able to gather enough evidence to support the second hypothesis that sticky erythrocytes obstruct blood flow in brain vessels, setting off the cascade of deleterious events leading to cerebral swelling.
To better understand the roots of brain swelling, the team not only relied on non-invasive infrared spectroscopy technique to study blood-flow dynamics in the brain, they also studied each child's brain via MRI as another method of obtaining a view of cerebral vasculature.
In addition to the 46 children with cerebral malaria who were examined in the research, an additional 33 children with uncomplicated malaria and 29 healthy children underwent imaging. Those with brain swelling had higher concentrations of hemoglobin in brain microvessels, which correlated with greater severity of brain swelling.
Malaria is a growing global health concern, even amid the arrival of promising new vaccines. The first immunization against malaria, called RTS,S developed by GlaxoSmithKline, was recommended by WHO nearly two years ago. A second immunization, R21/Matrix-M, recommended by WHO two weeks ago, was developed by Britain's University of Oxford. That vaccine will be ready for global distribution next year. Neither shot will beat the mosquito-borne infection into retreat anytime soon.
Climate change is driving the expansion of malaria's mosquito vectors across an increasingly broader geographical range. And an unexpected spate of malaria cases that didn't occur as a result of travel but emerged locally in several U.S. states this year, stirred public health officials who called for greater surveillance and vigilance.
Studies, such as those by Smith and her collaborators, will help scientists better understand a devastating complication of the infection and devise new ways to monitor it.
"These findings may help to elucidate the mechanisms responsible for brain swelling and coma in children with cerebral malaria," Smith concluded. "Continuous near-infrared spectroscopy monitoring could be used to further understand cerebral malaria pathophysiology, monitor its progression, and measure response to treatment."
More information: Rachel L. Smith et al, Increased brain microvascular hemoglobin concentrations in children with cerebral malaria, Science Translational Medicine (2023). DOI: 10.1126/scitranslmed.adh4293
© 2023 Science X Network