This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Does patient-surgeon gender concordance lead to lower patient mortality? Mostly no, research suggests
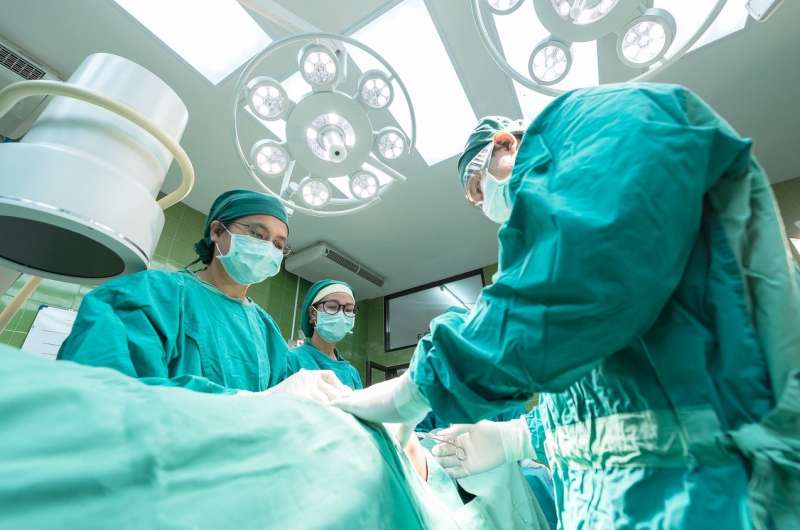
New research finds little evidence that post-surgical patient mortality is lower when patient and surgeon are the same gender.
While gender concordance has been shown to improve patient care in other health specialties, evidence has been limited when it comes to concordance between patient and surgeon. This study shows that gender concordance was associated with lower mortality for female patients, but higher mortality for male patients—patient mortality was the lowest for female patients treated by female surgeons, and the highest for male patients treated by male surgeons.
This study also investigated the impact of surgeon gender, and shows that female surgeons had slightly lower patient mortality than males for elective surgeries, but no gender difference for non-elective procedures.
The findings are published in the journal The BMJ on Nov. 22.
"It is important for patients to know that the quality of surgical care provided by female surgeons in the United States is equivalent to, or in some cases, slightly better than that provided by male surgeons," said senior author Dr. Yusuke Tsugawa, associate professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA. "Given that the difference in patient mortality between female and male surgeons was small, when choosing a surgeon, patients should take into account factors beyond the gender of the surgeon."
The researchers examined data for 2.9 million Medicare fee-for-service beneficiaries aged 65 years and older who underwent one of 14 surgeries between 2016 and 2019: abdominal aortic aneurysm repair, appendectomy, cholecystectomy, colectomy, coronary artery bypass surgery, knee replacement, hip replacement, hysterectomy, laminectomy or spinal fusion, liver resection, lung resection, prostatectomy, radical cystectomy, and thyroidectomy.
Of the participants, 1.2 million (41%) were male surgeon/patient pairs, 86,000 (3%) were female pairs, and 1.6 million (56%) were pairs of different genders (52,000, or 1.8%, were male patient/female surgeon and 1.5 million, or 54%, female patient/male surgeon). The outcome measure was death within 30 days of the procedure.
Adjusting for patient and surgeon characteristics and other factors, the researchers found that 30 day post-surgery mortality was 2.0% for male patient–male surgeon, 1.7% for male patient–female surgeon, 1.5% for female patient–male surgeon, and 1.3% for female patient–female surgeon pairs.
Study limitations include potential undetected confounders from Medicare claims data, an inability to account for contributory characteristics of other health care team members, and the possibility that the findings may not apply to younger patients.
But the findings could lead to a better understanding of processes that improve care for all patients, the researchers write. "Ongoing qualitative and quantitative research will better delineate how surgeon and patient gender, along with race and other aspects of shared identity, affect quality of care and outcomes after surgery," they write.
More information: Association between patient-surgeon gender concordance and mortality after surgery in the United States: retrospective observational study, The BMJ (2023). DOI: 10.1136/bmj-2023-075484