This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
New study offers hope for hundreds of thousands impacted each year by aggressive brain cancer
New research by the University of Sussex could help to increase life expectancy and improve treatment for an aggressive brain cancer, which impacts thousands of people every year in the UK, and hundreds of thousands worldwide.
In the study, published in the journal of Advanced Science, researchers have discovered that an understudied protein, called PANK4, is able to block cancer cells from responding to chemotherapeutic treatment for the highly intrusive brain cancer, glioblastoma.
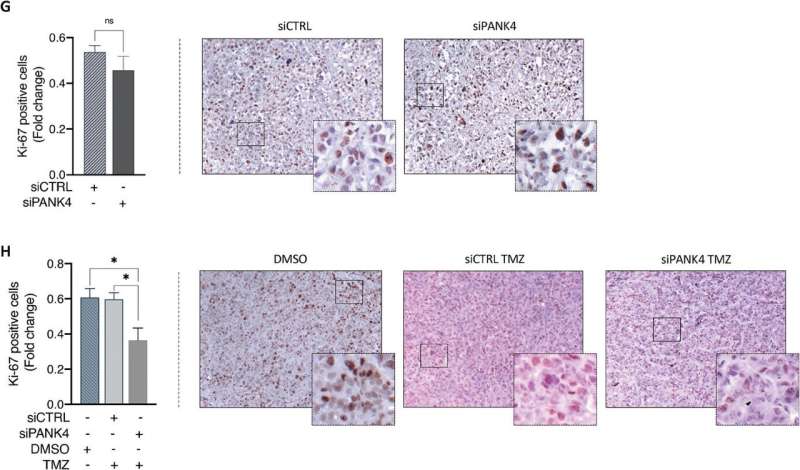
Scientists at Sussex have demonstrated that if the protein is removed, cancer cells respond better to the main chemotherapy drug used globally for the treatment of glioblastoma.
Prof Georgios Giamas, Professor of Cancer Cell Signalling at the University of Sussex, explains, "Glioblastoma is a devastating brain cancer, and researchers are working hard to identify ways to delay the progression of the disease and tackle cell resistance to treatment."
"As this is the first time that PANK4 has been linked to glioblastoma, the next step is to develop a drug targeting this protein to try to reverse chemo-resistance and restore sensitivity, ensuring that patients receive the best treatment and have better outcomes."
Glioblastoma is one of the most aggressive forms of brain cancer. Approximately 3,200 adults are diagnosed with the disease each year in the UK, and around 250,000—300,000 globally, with a best-case survival rate of just one to 18 months after diagnosis.
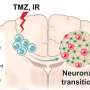
Following surgery to remove the tumor, glioblastoma patients are typically treated with radiation and the chemotherapeutic drug, temozolomide. Although patients initially respond well to the drug, the cancer cells quickly develop resistance to this treatment.
The University of Sussex scientists led an international research team to understand the possible reasons for this resistance, helping to guide future therapies to improve quality of life and increase life expectancy for those with glioblastoma.
The team identified a protein called PANK4, which, when removed from the cancer cells, can lead to the cell's death and saw patients better responding to temozolomide.
Linked to this, the researchers found that patients expressing high levels of the PANK4 protein had lower survival rates.
Dr. Viviana Vella, research fellow at the University of Sussex, explains, "There are a multitude of under-investigated proteins that may hold great potential for therapeutic intervention. Our study sheds light on this understudied protein, PANK4, unveiling a protective role in temozolomide-resistant cancer cells. Ultimately, PANK4 depletion represents a vulnerability that can now be exploited to restore sensitivity to the drug and improve treatment."
This study contributes to a body of research from the Sussex researchers, which focuses on the early diagnosis and treatment of glioblastoma.
The research group now hopes to develop a drug to reverse chemo-resistance and improve the outlook for patients.
More information: Viviana Vella et al, Kinome‐Wide Synthetic Lethal Screen Identifies PANK4 as a Modulator of Temozolomide Resistance in Glioblastoma, Advanced Science (2024). DOI: 10.1002/advs.202306027