This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
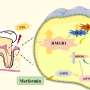
Researchers reveal how diabetes weakens gum defense
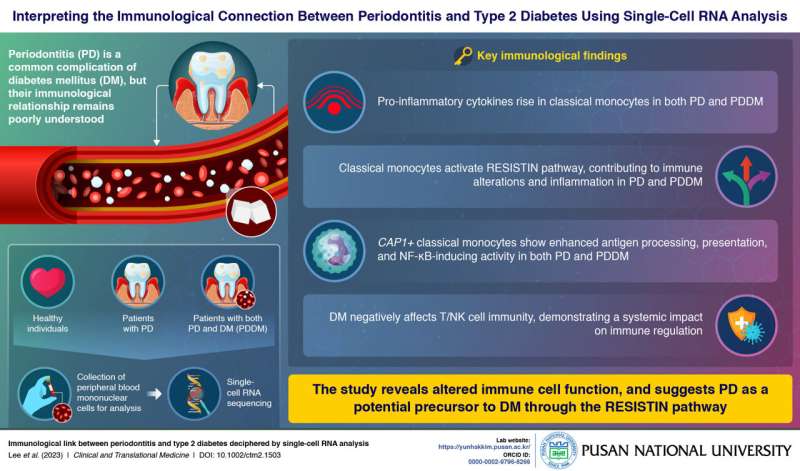
Periodontitis (PD) is a common complication in individuals with diabetes mellitus (DM). Despite the profound implications for overall health, the complex bidirectional relationship between them lacks a comprehensive understanding so far, leaving the precise nature of their immunological connection inadequately understood. Prior studies focusing on local immune responses in gingival tissue fall short of capturing the systemic immunological relationship.
In an innovative study, researchers from the Republic of Korea have investigated the relationship between periodontitis (PD) and diabetes mellitus (DM). Led by Assistant Professor Yun Hak Kim from Pusan National University, the study employs pioneering single-cell RNA analysis and digs into the immune dynamics at the cellular level.
This recent study was published in Clinical and Translational Medicine. Dr. Kim says, "Our study promises to transform our understanding of the complex interplay between these two prevalent health conditions and sheds light on the systemic impact of these conditions, offering a potential avenue for targeted interventions."
But what exactly is this immunological link?
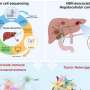
The study, conducted on a diverse group that included healthy individuals as well as patients with periodontitis (PD) and those with both PD and type 2 diabetes mellitus (PDDM), utilized single-cell RNA sequencing to explore the systemic immunological connections between PD and DM. The researchers methodically analyzed peripheral blood mononuclear cells by single-cell RNA sequencing, revealing transcriptomic characteristics and cell interactions.
The study identified pro-inflammatory cytokines rise in classical monocytes in both PD and PDDM groups. Further analysis revealed the influence of DM on T lymphocyte counts. CD4+ effector T cells exhibited reduced activation under DM conditions, indicating a broader systemic impact on immune regulation.
The compromised functions of CD8+ T cells and natural killer (NK) cells in the presence of both PD and DM further highlight the intricate immune changes occurring at the cellular level.
The RESISTIN pathway, known for its association with insulin resistance, was found to be intensified in both PD and PDDM groups, primarily involving classical monocytes. This discovery adds a crucial piece to the puzzle, suggesting a shared intercellular pathway that contributes to the complex PD-DM relationship.
The discovery of RESISTIN in the blood of patients with periodontitis but without underlying diseases highlights its role in inflammation and its potential as a therapeutic target to reduce diabetes risk in patients with PD. The outcomes point to significant immune alterations in patients with both PD and DM, emphasizing the potential role of PD as a precursor to diabetes.
Dr. Kim remarks, "Our study not only highlights the specific immune alterations associated with PD and DM but also underscores the shared pathways that intensify in the presence of both conditions."
"Leveraging the findings from our research, incorporating supplementary therapies for PD can facilitate glycemic control and reduce the likelihood of developing DM. Recognizing the capacity of PD to impact the susceptibility and handling of DM holds significant implications for health care, studies, public health, and the holistic welfare of individuals."
In conclusion, this research provides a first-of-its-kind immunological explanation for the complex association between periodontitis and type 2 diabetes mellitus. The use of single-cell RNA analysis has uncovered cellular-level immune changes, offering a new perspective on the systemic impact of these prevalent health conditions. The study not only advances our scientific understanding but also lays the foundation for potential interventions aimed at diminishing the risk and impact of diabetes in individuals with periodontitis.
More information: Hansong Lee et al, Immunological link between periodontitis and type 2 diabetes deciphered by single‐cell RNA analysis, Clinical and Translational Medicine (2023). DOI: 10.1002/ctm2.1503