This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Worse survival rates, different care for cancer patients who live further from the hospital in Scotland
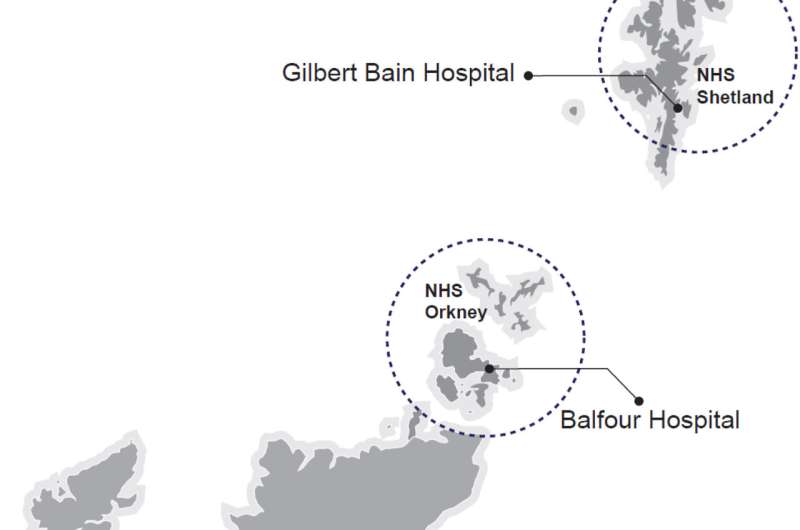
Patients who live further away from cancer centers are likely to receive different care and experience worse outcomes than those who live closer according to new research on patients in the north-east of Scotland and the Northern Isles. This is despite patients from further away being referred and diagnosed as quickly as people close to the center.
The study, published in the journal Health & Place, calls for 'better configuration of cancer services' across Scotland to address disparities in cancer care.
Professor Peter Murchie, Clinical Chair in Academic Primary Care at the University, who led the research alongside colleagues from NHS Grampian, investigated the relationship between distance to travel to the main cancer center with hospital appointments and admissions, and the patients' survival one-year after diagnosis.
The team found that those living in Orkney and Shetland spent more time in hospital and attended fewer oncology outpatient appointments. This was associated with a higher risk of death within a year of diagnosis compared to their mainland dwelling counterparts.
In contrast, patients on the mainland who had longer traveling times also spent more time in hospital but had more oncology outpatient appointments, and in their case, there was no increased risk of death within a year of diagnosis.
The data also showed that when patients who lived remotely had an emergency cancer admission, they were more likely to die within the first year.
However, longer traveling times or living on an island did not increase the likelihood of emergency admission for cancer or affect the length of time to first emergency cancer admission.
Dr. Melanie Turner, Advanced Research Fellow at the University, analyzed data from the NASCAR database collected from more than 17,000 patients diagnosed with one of eight solid cancer types over 10 years, from 2007 to 2017. The patients lived in north-east Scotland—an area covered by NHS Grampian, NHS Orkney and NHS Shetland health boards. Island patients made up 8% of the patients in the study.
Further analysis of factors that may influence survival found that it cannot be explained by age, type of treatment, socioeconomic status, non-cancer related co-morbidities or metastatic cancer. They did find a trend towards a positive effect of involvement of the oncology team where more oncology outpatient appointments reduced the risk. The team are now working to establish whether there is a difference in the treatment choices made by people living in the islands.
Dr. Turner explains, "The aim of this and future research is to ensure that decisions on cancer treatment and care following diagnosis are not based on difficulties in accessing health care facilities due to a high travel burden for patients. "
Dr. Leslie Samuel, Consultant Oncologist in NHS Grampian and Honorary Clinical Senior Lecturer at the University explains, "We already know that there is a difference in outcomes between urban and rural patients in North East Scotland, one marked difference being the paradox that while rural patients, with longer traveling times, tend to get a diagnosis and start treatment more promptly, their one year survival rate tends to be poorer.
"Research giving a better understanding of why these differences occur should enable the health service to not only review how cancer services are organized but also how this affects decisions patients make about treatment. In particular the 'time toxicity' for those patients with advanced disease and a higher travel burden."
Dr. Kirsty Brightwell, NHS Shetland Medical Director added, "NHS Shetland welcomes any research that shines a light on the issues for our population. This study looks at data from 2007 to 2017 and a lot has changed since then, not least of all the changes put in place during the pandemic.
"We continue to work closely with colleagues in NHS Grampian to improve services and deliver as much as we can as close to people's homes as possible while maintaining the quality of their experience and outcomes."
Dr. Louise Wilson, Director of Public Health at NHS Orkney said, "Our cancer care is delivered in partnership with the specialists in NHS Grampian and supporting patients to make the best treatment choice for their situation is important. More therapies are becoming available locally and we will work with NHS Grampian to get the best possible outcomes for our patients."
Professor Peter Murchie concluded, "It is essential that we continue to ensure equitable cancer care across all of Scotland's geography. This research is a good step forward in beginning to unpick the complex mechanisms underlying poorer outcomes for our rural cancer patients."
More information: Melanie Turner et al, The impact of travel time to cancer treatment centre on post-diagnosis care and mortality among cancer patients in Scotland, Health & Place (2023). DOI: 10.1016/j.healthplace.2023.103139