This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Developing research into mpox infections
A study, "Mpox infection protects against re-challenge in rhesus macaques," published in Cell, leads researchers to believe that the successful development of a mpox (previously known as monkeypox) vaccine may prevent humans from falling ill if they were to contract the disease.
The study has continued in the Martinot Lab at Cummings School of Veterinary Medicine at Tufts University by a team of faculty and students researching the mpox virus in endometrial tissues to raise awareness of the potential increased risk of mpox virus for women.
Dr. Amanda Martinot, assistant professor in the Departments of Infectious Disease and Global Health and Comparative Pathobiology at Cummings School, performed pathology studies for the original project. The work was a collaboration of several professionals, led by Dr. Dan Barouch, director of the Center for Virology and Vaccine Research at Beth Israel Deaconess Medical Center, a teaching hospital of Harvard Medical School.
Dr. Martinot completed her pathology training and earned her Ph.D. from Harvard University, where she studied the microbiology of tuberculosis infection at the Harvard School of Public Health. She then pursued training in immunology and vaccinology as a post-doctoral fellow in Dr. Barouch's lab and has since served as a pathologist for several of his research projects.
"Reading pathology is a large part of my work, both in my research lab and as a professional," says Dr. Martinot. "Dr. Barouch conducts non-human primate research, primarily efficacy studies, which aim to determine if there is a good chance that a vaccine might work."
One method of testing is to ask whether contracting a disease through natural infection will protect an individual against getting the same disease again. If natural infection protects against repeat infections, that is a good indication that a vaccine might help protect against that disease, according to Dr. Martinot.
A similar strategy was followed when Dr. Martinot was part of a team that investigated the Zika virus—a virus spread mainly via mosquito bites, that can lead to birth defects—and COVID-19. In both instances, rhesus macaque monkeys were used to understand disease pathogenesis and potential for vaccine protection.
According to National Primate Research Centers, rhesus share about 93 percent of their genes with humans and have been used in nearly every area of biomedical research. When it comes to understanding human immune responses to infections and vaccines, they can provide highly applicable information that can help physicians and scientists solve human health problems.
"We challenge the animals with the virus, then look to see whether a re-challenge would protect them against the subsequent infection," Dr. Martinot says. "That requires pathologists to look at animal tissues and determine if they are protected from both viral replication and disease manifestation."
An outbreak of mpox in 2022–2023 led to 80,000 cases in 110 countries worldwide, including some 30,000 cases in the United States, earning mpox a designation from the World Health Organization as a public health emergency of internal concern. It was believed to spread mostly through sexual and skin-to-skin contact.
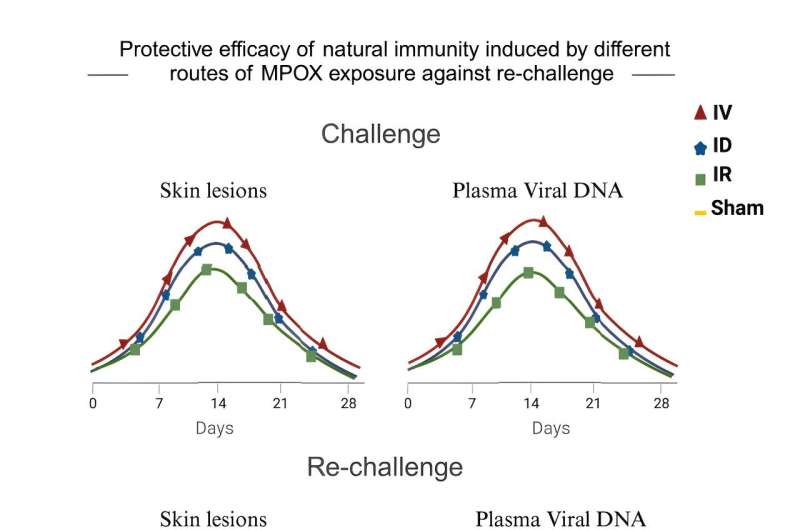
The study inoculated 18 adult rhesus macaques with mpox and then evaluated their humoral and cellular immune responses after two and four weeks.
"We learned that if an animal is previously infected with mpox, they will be protected against a subsequent infection," says Dr. Martinot. "This indicates that if we have a vaccine for mpox, we could probably prevent people from getting sick as well."
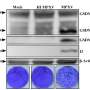
Mpox attacks the body like a vesicular disease, such as smallpox, which causes skin lesions. As part of the original study, Dr. Martinot evaluated whether a first infection or second infection leads to the characteristic "pox" skin lesions.
"Monkeys that had one infection did develop skin lesions," she says. "And we noticed that the animals had several other lesions that have not been previously described in people, so that's one of the things that I'm working to try to understand." Monkeys that had a second infection did not develop the classic pox skin lesions, and this corresponded to their strong immune responses against the virus.
Dr. Martinot explained that pox viruses are quite infectious, and therefore concern was high when the disease emerged. While affirming that mpox infections have quieted down, Dr. Martinot is optimistic despite the continuing threat.
"We know that the vaccine for smallpox also protects against mpox," she says. "In general, I think people should be less concerned about mpox, because we have the tools, and we know how to make a vaccine that will protect vulnerable populations or people at risk for this disease."
According to the Centers for Disease Control and Prevention, two vaccines are in use against mpox. JYNNEOS has been approved for the prevention of mpox and smallpox and is the main vaccine used in the U.S. ACAM2000 is approved for immunization against smallpox and made available for use against mpox under an expanded access protocol.
During the course of the study, researchers detected the mpox virus in the skin, cervix, uterus, and periovarian endometriosis lesions in a female rhesus macaque with severe endometriosis (when endometrial tissue is found outside the uterus). This finding indicated that women may be at higher risk of mpox if pregnant or suffering from endometriosis. Dr. Martinot felt this warranted further study and pulled in a team at Cummings School.
Josh Hall is first author on the new research manuscript, recently submitted for publication. He began working with Dr. Martinot almost two years ago in the veterinary student summer research program and has been a dedicated member of her team ever since. For the mpox research project, Hall developed complex tissue staining protocols and then scanned images for image analysis. This allowed the team to determine what cell types in the reproductive tract were infected with pox virus.
"The fact that we found mpox lesions in the female reproductive tract was an interesting case," says Hall. "Mpox is mostly seen in men, but it's just as infectious in women. We thought this was a strong enough story to get the information out there, to help both animal researchers and doctors have an understanding of the pathogenesis."
Jingyi (Jenny) Li began working in the Martinot Lab during her second year at Cummings School after taking Dr. Martinot's digital pathology elective. She will begin residency at the University of Illinois for anatomic pathology after she graduates this spring. She was responsible for tissue trimming, staining, and histopathology analysis in the mpox research studies.
Li says, "Description of mpox lesions in the reproductive tract of women is limited, and assessing the lesions in human patients is difficult and invasive. The rhesus macaque is a useful model since it has a similar reproductive anatomy to humans. This case report will help us understand mpox lesions in the reproductive tract and raise awareness of potential similar lesions in human patients."
Dr. Claire Lyons is an anatomic pathologist in the Martinot Lab and the Comparative Pathology and Genomics Shared Resource at Cummings School. After earning her DVM at Cummings School, she completed her postdoctoral training and fellowship in comparative pathology at Johns Hopkins University and MIT. She analyzes pathology specimens for projects involving mpox, COVID-19, and tuberculosis in the Martinot Lab.
For the mpox study, Dr. Lyons ensured all the desired stains had been run, and slides had been scanned, and assisted the students in writing descriptions and analyzing the slides, looking for inflammatory cells that indicate the mpox virus in a tissue that's not expected.
"No research has been published for human women showing monkeypox in the reproductive tract anywhere other than the outside surface of the cervix," says Dr. Lyons. "This research brings attention to the potential for the virus to travel outside of the uterus. Endometriosis is such a prevalent condition and can spread through the abdomen. Mpox might impact tissues that endometrial lesions are attached to."
The students and researchers in the Martinot Lab put forth these findings as a team.
"Working with students has been great—they're excited and really want to figure out exactly what's happening, to learn all the techniques, poke around with software. They bring so much energy," says Dr. Lyons. "I like being on a team looking for answers to big burning questions, to help people and animals."
More information: Malika Aid et al, Mpox infection protects against re-challenge in rhesus macaques, Cell (2023). DOI: 10.1016/j.cell.2023.08.023