This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
proofread
Researchers introduce ten-minute breath test to monitor antibiotic concentrations

Exhaled breath may be very promising alternative to blood for the therapeutic monitoring of antibiotics, the ESCMID Global Congress (formerly ECCMID) in Barcelona, Spain (27-30 April) will hear.
Therapeutic drug monitoring (TDM) is used to monitor antibiotic concentrations in patients with severe infections and in patients in intensive care units. These patients may metabolize drugs differently and so may not respond to conventional doses of antibiotics (they require higher doses) or be more likely to develop toxic side effects (they require lower doses). The TDM results allow the dosage to be tailored to their needs.
"Currently, we use blood samples to do this," says lead researcher Dr. Sarah Dräger, of the Division of Internal Medicine, University Hospital Basel, Basel, Switzerland. "But the collection of blood is an invasive, time- and resource-consuming technique and leads to discomfort in patients. It takes several hours or even days to get results, depending on the antibiotic tested, and so the results may come too late to guide the treatment of some of the sickest patients.
"Using exhaled breath has several advantages: It is non-invasive, it is easy to collect and it is not associated with discomfort to the patient. It also has the potential to decrease the turnaround time, especially when combined with real-time analyses, when it could provide results in as little as ten minutes. It is already used to monitor other drugs, such as antiseizure medicines, and we wanted to explore its potential in monitoring antibiotics."
Dr. Dräger and Professor Pablo Sinues, head of the Translational Medicine Research Group at the University Children's Hospital of Basel, conducted a prospective, single-center proof-of-concept study involving 10 patients (median age 63 years, 54.5% female) who received intravenous antibiotic treatment in 2022 or 2023.
They were being treated for respiratory infections (n=3), intravascular infections (n=3), abdominal infections (n=2), urinary tract infection (n=1) or skin and soft tissue infection (n=1) with meropenem (n=3), piperacillin/tazobactam (n=3), cefazolin (n=2), flucloxacillin (n=1) or ciprofloxacin (n=1).
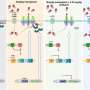
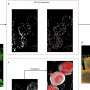
Mass spectrometry was used to analyze samples of exhaled breath for exogeneous metabolites (breakdown products of the antibiotic) and endogenous metabolites (breakdown products from the body that are affected by the antibiotic).
With four antibiotics—meropenem, cefazolin, flucloxacillin and ciprofloxacin—it was possible to detect differences in the levels of specific metabolites. With one antibiotic, piperacillin/tazobactam, no clear signal was detected.
The hope is that by measuring levels of these metabolites it will be possible to monitor antibiotic concentrations without taking blood samples.
Dr. Dräger says, "We were able to detect antibiotic-specific metabolites in exhaled breath in patients treated with antibiotics in four out of five antibiotics investigated.
"We aim to confirm these very promising results in a larger cohort of patients, as well as look at how they relate to blood plasma concentrations of antibiotics and patient outcomes."
More information: Abstract P2422 at the ESCMID Global Congress (formerly ECCMID).