This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Income and regional disparities dictate how young people use health care services
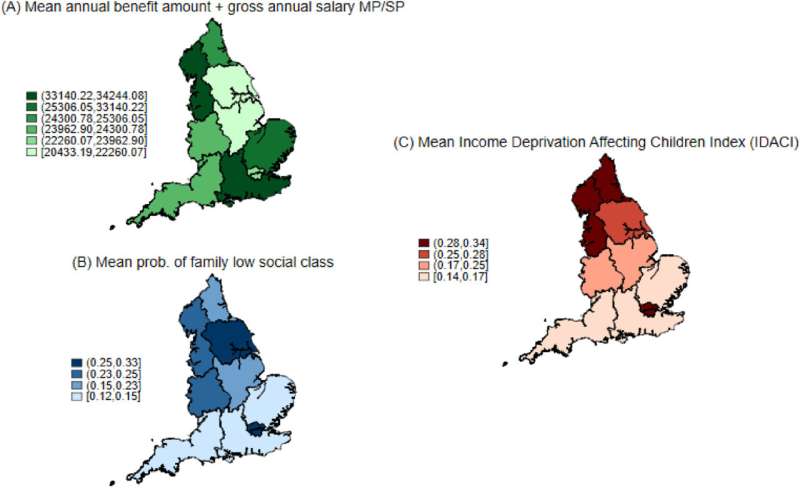
There is a stark contrast in how young people access health care, depending on their income and where they live.
According to a new study from Imperial College Business School, people aged 14 to 17 living in more affluent areas have easier and faster access to outpatient care, including mental health and dental services.
By contrast, those in more deprived areas struggle to access preventative health care. They face longer waiting times and are more likely to cancel or not attend outpatient appointments (though the study does not explore the reasons for this). This means their health is more likely to worsen, making them more reliant on emergency care when they need urgent medical treatment, according to the study.
The research, published in Social Science & Medicine, used data from Next Steps on people born in England in 1989–1990. Researchers interviewed more than 13,000 participants at age 14–15 and more than 11,000 at age 16–17. They then linked more than 4,000 of the participants to their hospital records when they turned 25, providing data about their use of health care services since their teenage years.
"Our study uncovers a stark contrast in health care usage between adolescents from income-deprived areas and those from wealthier areas," said Dr. Mario Martínez-Jiménez, Research Associate at Imperial's Center for Health Economics & Policy Innovation, and lead author of the study.
Although the study focused on a cohort of millennials (adults who are now in their 30s), the researchers say the findings are still relevant for today's adolescents who were more likely to struggle with their mental health during the COVID-19 pandemic.
"The disparity we found indicates a troubling scenario where poorer adolescents rely more on emergency care, potentially due to a lack of access to regular, preventative health care services. For today's teenagers, we believe this may have been exacerbated due to the COVID-19 pandemic and the effect of lockdowns on young people," Dr. Martínez-Jiménez explained.
Regional divide
The research shows how people's economic circumstances play a big role in how they experience health care during their adolescence.
The researchers quantified the relative impact on health and health care inequalities of circumstances beyond young people's control, such as their parents' socioeconomic status and where they live, and lifestyle habits within their control, such as smoking, drinking and playing sports.
While lifestyle factors were found to influence the situation, the study found that regional differences and parents' socioeconomic status were likely to have the biggest impact on young people's access to hospital services.
This geographical context is important, given the findings show that young people living in more affluent areas tend to face shorter waiting times for outpatient appointments. According to the study, these early-intervention specialist appointments prevent health issues developing into medical emergencies, and difficulty accessing them leaves young people in more deprived areas more reliant on accident and emergency departments.
Emergency services
The researchers also identified an inequality of access to accident and emergency services. They found that emergency services in more deprived areas were more likely to be overwhelmed and under-resourced than in wealthier areas.
This leads to young people facing longer waiting times due to greater demand and lower resources in deprived areas, potentially exacerbating inequalities between more and less deprived areas. This is in line with more recent Census data showing that accident and emergency attendance increases with the level of deprivation people experience.
"Given that young people from poorer backgrounds face overall worse health, this means there is a risk they could get caught in a cycle of poor health and insufficient treatment," Dr. Martínez-Jiménez said.
"Without effective measures and policies to address this, the U.K. is at risk of failing to uphold the core principle of providing equal health care services to all citizens based on their level of need," he said.
More information: Mario Martínez-Jiménez et al, Socioeconomic deprivation, health and healthcare utilisation among millennials, Social Science & Medicine (2024). DOI: 10.1016/j.socscimed.2024.116961