Risk of newborn death cut in half when pregancy lasts 39 weeks, new research finds
Adding just a few more weeks of pregnancy can cut a newborn's risk of death in half – even if the pregnancy has reached "term" -- adding more evidence to the argument that continuing a pregnancy to at least 39 weeks is crucial to a baby's health.
The research by a team of investigators from the March of Dimes, the National Institutes of Health and the US Food and Drug Administration found that although the overall risk of death is small, it more than doubles for infants born at 37 weeks of pregnancy, when compared to babies born at 40 weeks, for all races and ethnicities.
In 2006, the infant mortality rate was 1.9 for every 1,000 live births for babies born at 40 weeks of pregnancy. The mortality rate increased to 3.9 per 1,000 when a baby was born just a few weeks earlier at 37 weeks of pregnancy, the study found.
"There is the perception that babies born between 37 and 41 weeks of pregnancy are all born healthy. But this study confirms that even babies born just a week or two early have an increased risk of death," said Alan R. Fleischman, MD, senior vice president and medical director at the March of Dimes. "It is clear, that regardless of race or ethnicity, every additional week of pregnancy is critical to a baby's health."
While there are times when medical reasons require a baby to be delivered early, an early elective delivery is harmful to a baby and should never be scheduled before 39 or 40 weeks of pregnancy.
The study titled: "Term pregnancy: a period of heterogeneous risk for infant mortality," was led by Uma M. Reddy, MD, MPH of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, of the National Institutes of Health, was published in Obstetrics & Gynecology, Vol. 117, No. 6, June 2011.
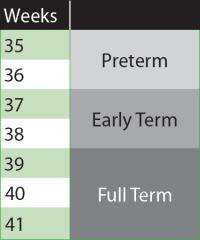
Preterm birth is less than 37 completed weeks of pregnancy. Until recently, babies born after 37 weeks of pregnancy were evaluated as a single, homogenous group, the March of Dimes says. The investigators found that early term infants had higher infant and neonatal mortality rates when compared to full term infants for every year from 1995 to 2006. Neonatal infant mortality rates were highest for infants born at 37 weeks of pregnancy, and declined for each additional week until 40 weeks, which had the lowest neonatal death rates. The trend was the same for all races and ethnicities. However, of the infants in the study non-Hispanic black infants had the highest infant mortality rates and the smallest declines at 37 and 38 weeks, the researchers said.
"Although infant mortality rates overall improved in the past decade, rates for non-Hispanic blacks babies born at 37 or 38 weeks of pregnancy remain unacceptably higher than other racial and ethnic groups," said Dr. Reddy. "Our results indicate that intervention programs are needed for this high-risk group, as is additional research to understand why non-Hispanic black infants are less likely than other groups to live to celebrate their first birthday."













